Hypercortisolemia Recurrence in Cushing's Disease; a Diagnostic Challenge
- PMID: 31787930
- PMCID: PMC6856050
- DOI: 10.3389/fendo.2019.00740
Hypercortisolemia Recurrence in Cushing's Disease; a Diagnostic Challenge
Abstract
Cushing's disease recurrence following successful pituitary surgery is common and merits prompt and careful diagnosis, as untreated hypercortisolism leads to increased morbidity and mortality. However, an established recurrence definition has not been forthcoming. This poses a diagnostic challenge especially early in the course of returning hypercortisolemia and/or in the presence of non-neoplastic hypercortisolemia. A late-night salivary cortisol (LNSC) test is the first test to reveal abnormal results, however, has limitations related to assay performance as well as individual patient variability. Dexamethasone suppression tests and 24-h urinary free cortisol (UFC) results are next to reveal abnormal results. Other tests including, corticotropin-releasing hormone (CRH) stimulation test and combined CRH-dexamethasone test, as well as desmopressin stimulation test with/without dexamethasone are also used, although, none have proven to be the preeminent diagnostic test for recurrence determination. There is a possible role for these tests in predicting recurrence in patients who have experienced remission, though, this also remains challenging due to lack of established cutoff values. This article details and summarizes evidence about different diagnostic tests currently used to diagnose and predict Cushing's disease recurrence.
Keywords: Cushing; Cushing's disease; Cushing's syndrome; diagnostic testing; hypercortisolemia; recurrence; remission.
Copyright © 2019 Hinojosa-Amaya, Varlamov, McCartney and Fleseriu.
Figures

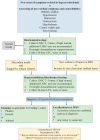
References
Publication types
LinkOut - more resources
Full Text Sources

