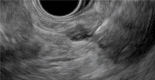
Endoscopic ultrasound-through-the-needle biopsy in pancreatic cystic lesions: A large single center experience
- PMID: 31798774
- PMCID: PMC6875688
- DOI: 10.4253/wjge.v11.i11.531
Endoscopic ultrasound-through-the-needle biopsy in pancreatic cystic lesions: A large single center experience
Abstract
Background: Establishing a diagnosis of pancreatic cystic lesions (PCLs) preoperatively still remains challenging. Recently, endoscopic ultrasound (EUS)-through-the-needle biopsy (EUS-TTNB) using microforceps in PCLs has been made available.
Aim: To assess the efficacy and safety of EUS-TTNB in the diagnosis of PCLs.
Methods: We retrospectively collected data of patients with PCLs who underwent both EUS-fine-needle aspiration (FNA) for cytology and EUS-TTNB at our institution since 2016. EUS-FNA for cytology was followed by EUS-TTNB in the same session. Evaluation of the cyst location, primary diagnosis, adverse events, and comparison between the cytologic fluid analyses and histopathology was performed. Technical success of EUS-TTNB was defined as visible tissue present after biopsy. Clinical success was defined as the presence of a specimen adequate to make a histologic or cytologic diagnosis.
Results: A total of 56 patients (mean age 66.9 ± 11.7, 53.6% females) with PCLs were enrolled over the study period. The mean cyst size was 28.8 mm (12-85 mm). The EUS-TTNB procedure was technically successful in all patients (100%). The clinical success rate using EUS-TTNB was much higher than standard EUS-FNA, respectively 80.4% (45/56) vs 25% (14/56). Adverse events occurred in 2 patients (3.6%) who developed mild pancreatitis that resolved with medical therapy. Using TTNB specimens, 23 of 32 cases (71.9%) with intraductal papillary mucinous neoplasm were further differentiated into gastric type (19 patients) and pancreaticobiliary type (4 patients) based on immunochemical staining.
Conclusion: EUS-TTNB for PCLs was technically feasible and had a favorable safety profile. Furthermore, the diagnostic yield for PCLs was much higher with EUS-TTNB than standard EUS-FNA cytology and fluid carcinoembryonic antigen. EUS-TTNB should be considered as an adjunct to EUS-FNA and cytologic analysis in the diagnosis and management of PCLs.
Keywords: Biopsy; Cyst fluid; Endoscopic ultrasound; Endoscopic ultrasound-guided fine needle aspiration; Pancreatic cyst lesion.
©The Author(s) 2019. Published by Baishideng Publishing Group Inc. All rights reserved.
Conflict of interest statement
Conflict-of-interest statement: No financial support was received from the company of microforceps to conduct this study. Dr Samarasena is a consultant to US Endoscopy. None of the other authors have any relevant conflicts of interest.
Figures
References
-
- Ketwaroo GA, Mortele KJ, Sawhney MS. Pancreatic Cystic Neoplasms: An Update. Gastroenterol Clin North Am. 2016;45:67–81. - PubMed
-
- Lee KS, Sekhar A, Rofsky NM, Pedrosa I. Prevalence of incidental pancreatic cysts in the adult population on MR imaging. Am J Gastroenterol. 2010;105:2079–2084. - PubMed
-
- Kromrey ML, Bülow R, Hübner J, Paperlein C, Lerch MM, Ittermann T, Völzke H, Mayerle J, Kühn JP. Prospective study on the incidence, prevalence and 5-year pancreatic-related mortality of pancreatic cysts in a population-based study. Gut. 2018;67:138–145. - PubMed
-
- Scheiman JM, Hwang JH, Moayyedi P. American gastroenterological association technical review on the diagnosis and management of asymptomatic neoplastic pancreatic cysts. Gastroenterology. 2015;148:824–48.e22. - PubMed