Antibiotic-impregnated bone cement for preventing infection in patients receiving primary total hip and knee arthroplasty: A meta-analysis
- PMID: 31804314
- PMCID: PMC6919433
- DOI: 10.1097/MD.0000000000018068
Antibiotic-impregnated bone cement for preventing infection in patients receiving primary total hip and knee arthroplasty: A meta-analysis
Abstract
Background: Surgical-site infections after primary total joint arthroplasty (TJA) are a significant issue. Antibiotic-impregnated bone cement (AIBC) has been widely used for the treatment of infected joints, but routine use of AIBC in primary TJA remains controversial. In this systematic review, we evaluated the efficacy of AIBC in reducing surgical-site infections after primary TJA.
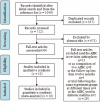
Methods: We systematically searched Pubmed, EMbase, Cochrane Library, CMB, CNKI, and WanFang Data for studies (published until June 1, 2019) evaluating AIBC use in reducing infection rates. Two reviewers independently screened the literature according to inclusion and exclusion criteria, extracted data, and assessed the methodological quality of included studies. Meta-analysis was performed using Review Manager 5.3 software. The registration number is CRD42017078341 in PROSPERO.
Results: In total, 10 studies were included, resulting in a sample size of 13,909 arthroplasty cases. The overall pooled data demonstrated that, compared with systemic antibiotics, AIBC was more effective in decreasing deep infection rates (odds ratio [OR] = 0.35, 95% confidence interval [CI] = 0.14-0.89, P = .030), although there were higher superficial infection rates with AIBC (OR = 1.53, 95% CI = 1.11-2.11, P = .010). Compared to systemic antibiotics alone, AIBC with systemic antibiotics significantly decreased deep infection rates (OR = 0.55, 95% CI = 0.41-0.75, P = .0001) but there was no difference in superficial infection rates (OR = 1.43, 95% CI = 0.81-2.54, P = .220). In the subgroup analysis, both randomized controlled trials and cohort studies had reduced deep infection rates after primary TJA (OR = 0.61, 95% CI = 0.37-0.99, P = .050 and OR = 0.49, 95% CI = 0.34-0.70, P = .0001, respectively). AIBC decreased deep infection rates in both total hip and knee arthroplasty (OR = 0.25, 95% CI = 0.12-0.52, P = .0002 and OR = 0.62, 95% CI = 0.45-0.87, P = .005, respectively). Deep infection rates were significantly decreased by AIBC with gentamicin (OR = 0.31, 95% CI = 0.20-0.49, P < .00001) but unaffected by AIBC with cefuroxime (OR = 0.35, 95% CI = 0.10-1.20, P = .100). Deep infection rates in the AIBC and control groups were similar when laminar airflow was applied to the operating room (OR = 0.90, 95% CI = 0.60-1.35, P = .620); however, without laminar airflow, the efficacy of AIBC in decreasing deep infection rates was significantly higher than that of control group (OR = 0.21, 95% CI = 0.08-0.59, P = .003).
Conclusions: AIBC may significantly decrease deep infection rates after primary total hip and knee arthroplasty, with or without systemic antibiotics.
Conflict of interest statement
The authors have no conflicts of interest to disclose.
Figures






Similar articles
-
A systematic review and meta-analysis of antibiotic-impregnated bone cement use in primary total hip or knee arthroplasty.PLoS One. 2013 Dec 12;8(12):e82745. doi: 10.1371/journal.pone.0082745. eCollection 2013. PLoS One. 2013. PMID: 24349353 Free PMC article.
-
Effect of Antibiotic-Impregnated Bone Cement in Primary Total Knee Arthroplasty.J Arthroplasty. 2019 Sep;34(9):2091-2095.e1. doi: 10.1016/j.arth.2019.04.033. Epub 2019 Apr 22. J Arthroplasty. 2019. PMID: 31109755
-
Comprehensive meta-analysis of antibiotic-impregnated bone cement versus plain bone cement in primary total knee arthroplasty for preventing periprosthetic joint infection.Chin J Traumatol. 2022 Nov;25(6):325-330. doi: 10.1016/j.cjtee.2022.06.001. Epub 2022 Jun 9. Chin J Traumatol. 2022. PMID: 35717367 Free PMC article.
-
Efficacy of antibiotic-impregnated cement in total hip replacement.Acta Orthop. 2008 Jun;79(3):335-41. doi: 10.1080/17453670710015229. Acta Orthop. 2008. PMID: 18622836
-
Antibiotic bone cement's effect on infection rates in primary and revision total knee arthroplasties.World J Orthop. 2017 Dec 18;8(12):946-955. doi: 10.5312/wjo.v8.i12.946. eCollection 2017 Dec 18. World J Orthop. 2017. PMID: 29312854 Free PMC article.
Cited by
-
Study protocol: The DAICY trial-dual versus single-antibiotic impregnated cement in primary hemiarthroplasty for femoral neck fracture-a register-based cluster-randomized crossover-controlled trial.Acta Orthop. 2022 Oct 5;93:794-800. doi: 10.2340/17453674.2022.4819. Acta Orthop. 2022. PMID: 36200646 Free PMC article.
-
The use of antibiotic-loaded bone cement and systemic antibiotic prophylactic use in 2,971,357 primary total knee arthroplasties from 2010 to 2020: an international register-based observational study among countries in Africa, Europe, North America, and Oceania.Acta Orthop. 2023 Aug 9;94:416-425. doi: 10.2340/17453674.2023.17737. Acta Orthop. 2023. PMID: 37565339 Free PMC article.
-
In vitro elution characteristics of gentamicin-impregnated Polymethylmethacrylate: premixed with a second powder vs. liquid Lyophilization.BMC Musculoskelet Disord. 2021 Jan 4;22(1):5. doi: 10.1186/s12891-020-03923-w. BMC Musculoskelet Disord. 2021. PMID: 33397342 Free PMC article.
-
Prevention of Prosthetic Joint Infection: From Traditional Approaches towards Quality Improvement and Data Mining.J Clin Med. 2020 Jul 11;9(7):2190. doi: 10.3390/jcm9072190. J Clin Med. 2020. PMID: 32664491 Free PMC article. Review.
-
Association of Acute Kidney Injury With Antibiotic Loaded Cement Used for Treatment of Periprosthetic Joint Infection.J Arthroplasty. 2023 Dec;38(12):2704-2709.e1. doi: 10.1016/j.arth.2023.05.061. Epub 2023 Jun 4. J Arthroplasty. 2023. PMID: 37279850 Free PMC article.
References
-
- Merollini KM, Crawford RW, Whitehouse SL, et al. Surgical site infection prevention following total hip arthroplasty in Australia: a cost-effectiveness analysis. Am J Infect Control 2013;41:803–9. - PubMed
-
- Vasso M, Schiavone Panni A, De Martino I, et al. Prosthetic knee infection by resistant bacteria: the worst-case scenario. Knee Surg Sports Traumatol Arthrosc 2016;24:3140–6. - PubMed
-
- Mayne AIW, Davies PSE, Simpson JM. Antibiotic treatment of asymptomatic bacteriuria prior to hip and knee arthroplasty; a systematic review of the literature. - PubMed
-
- Cui Q, Mihalko WM, Shields JS, et al. Antibiotic-impregnated cement spacers for the treatment of infection associated with total hip or knee arthroplasty. J Bone Joint Surg Am 2007;89:871–82. - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical

