Effect of True and Sham Acupuncture on Radiation-Induced Xerostomia Among Patients With Head and Neck Cancer: A Randomized Clinical Trial
- PMID: 31808921
- PMCID: PMC6902763
- DOI: 10.1001/jamanetworkopen.2019.16910
Effect of True and Sham Acupuncture on Radiation-Induced Xerostomia Among Patients With Head and Neck Cancer: A Randomized Clinical Trial
Abstract
Importance: Radiation-induced xerostomia (RIX) is a common, often debilitating, adverse effect of radiation therapy among patients with head and neck cancer. Quality of life can be severely affected, and current treatments have limited benefit.
Objective: To determine if acupuncture can prevent RIX in patients with head and neck cancer undergoing radiation therapy.
Design, setting, and participants: This 2-center, phase 3, randomized clinical trial compared a standard care control (SCC) with true acupuncture (TA) and sham acupuncture (SA) among patients with oropharyngeal or nasopharyngeal carcinoma who were undergoing radiation therapy in comprehensive cancer centers in the United States and China. Patients were enrolled between December 16, 2011, and July 7, 2015. Final follow-up was August 15, 2016. Analyses were conducted February 1 through 28, 2019.
Intervention: Either TA or SA using a validated acupuncture placebo device was performed 3 times per week during a 6- to 7-week course of radiation therapy.
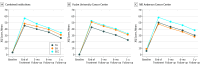
Main outcomes and measures: The primary end point was RIX, as determined by the Xerostomia Questionnaire in which a higher score indicates worse RIX, for combined institutions 1 year after radiation therapy ended. Secondary outcomes included incidence of clinically significant xerostomia (score >30), salivary flow, quality of life, salivary constituents, and role of baseline expectancy related to acupuncture on outcomes.
Results: Of 399 patients randomized, 339 were included in the final analysis (mean [SD] age, 51.3 [11.7] years; age range, 21-79 years; 258 [77.6%] men), including 112 patients in the TA group, 115 patients in the SA group, and 112 patients in the SCC group. For the primary aim, the adjusted least square mean (SD) xerostomia score in the TA group (26.6 [17.7]) was significantly lower than in the SCC group (34.8 [18.7]) (P = .001; effect size = -0.44) and marginally lower but not statistically significant different from the SA group (31.3 [18.6]) (P = .06; effect size = -0.26). Incidence of clinically significant xerostomia 1 year after radiation therapy ended followed a similar pattern, with 38 patients in the TA group (34.6%), 54 patients in the SA group (47.8%), and 60 patients in the SCC group (55.1%) experiencing clinically significant xerostomia (P = .009). Post hoc comparisons revealed a significant difference between the TA and SCC groups at both institutions, but TA was significantly different from SA only at Fudan University Cancer Center, Shanghai, China (estimated difference [SE]: TA vs SCC, -9.9 [2.5]; P < .001; SA vs SCC, -1.7 [2.5]; P = .50; TA vs SA, -8.2 [2.5]; P = .001), and SA was significantly different from SCC only at the University of Texas MD Anderson Cancer Center, Houston, Texas (estimated difference [SE]: TA vs SCC, -8.1 [3.4]; P = .016; SA vs SCC, -10.5 [3.3]; P = .002; TA vs SA, 2.4 [3.2]; P = .45).
Conclusions and relevance: This randomized clinical trial found that TA resulted in significantly fewer and less severe RIX symptoms 1 year after treatment vs SCC. However, further studies are needed to confirm clinical relevance and generalizability of this finding and to evaluate inconsistencies in response to sham acupuncture between patients in the United States and China.
Trial registration: ClinicalTrials.gov identifier: NCT01266044.
Conflict of interest statement
Figures
Comment in
-
Acupuncture-A Question of Culture.JAMA Netw Open. 2019 Dec 2;2(12):e1916929. doi: 10.1001/jamanetworkopen.2019.16929. JAMA Netw Open. 2019. PMID: 31808917 No abstract available.
References
-
- Eisbruch A, Ten Haken RK, Kim HM, Marsh LH, Ship JA. Dose, volume, and function relationships in parotid salivary glands following conformal and intensity-modulated irradiation of head and neck cancer. Int J Radiat Oncol Biol Phys. 1999;45(3):577-587. doi:10.1016/S0360-3016(99)00247-3 - DOI - PubMed
-
- Bertram U. Xerostomia: clinical aspects, pathology and pathogenesis. Acta Odontol Scand. 1967;25(suppl 49):1-126. - PubMed
Publication types
MeSH terms
Associated data
LinkOut - more resources
Full Text Sources
Medical
Research Materials

