Effects of Accessible Health Technology and Caregiver Support Posthospitalization on 30-Day Readmission Risk: A Randomized Trial
- PMID: 31810829
- PMCID: PMC7967033
- DOI: 10.1016/j.jcjq.2019.10.009
Effects of Accessible Health Technology and Caregiver Support Posthospitalization on 30-Day Readmission Risk: A Randomized Trial
Abstract
Introduction: Patients with chronic illness often require ongoing support postdischarge. This study evaluated a simple-to-use, mobile health-based program designed to improve postdischarge follow-up via (1) tailored communication to patients using automated calls, (2) structured feedback to informal caregivers, and (3) automated alerts to clinicians about urgent problems.
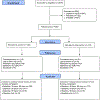
Methods: A total of 283 patients with common medical diagnoses, including chronic obstructive pulmonary disease, coronary artery disease, pneumonia, and diabetes, were recruited from a university hospital, a community hospital, and a US Department of Veterans Affairs hospital. All patients identified an informal caregiver or "care partner" (CP) to participate in their postdischarge support. Patient-CP dyads were randomized to the intervention or usual care. Intervention patients received weekly automated assessment and behavior change calls. CPs received structured e-mail feedback. Outpatient clinicians received fax alerts about serious problems. Primary outcomes were 30-day readmission rate and the combined outcome of readmission/emergency department (ED) use. Information about postdischarge outpatient visits, rehospitalizations, and ED encounters was obtained from medical records.
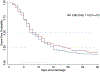
Results: Overall, 11.4% of intervention patients and 17.9% of controls were rehospitalized within 30 days postdischarge (hazard ratio [HR]: 0.59; 95% confidence interval [CI]: 0.31-1.11; p = 0.102). Compared to intervention patients with other illnesses, those with pulmonary diagnoses generated the most clinical alerts (p = 0.004). Pulmonary patients in the intervention group showed significantly reduced 30-day risk of rehospitalization relative to controls (HR: 0.31; 95% CI: 0.11-0.87; p = 0.026).
Conclusion: The CP intervention did not improve 30-day readmission rates overall, although post hoc analyses suggested that it may be promising among patients with pulmonary diagnoses.
Copyright © 2019. Published by Elsevier Inc.
Conflict of interest statement
Declaration of Conflicts of Interest: The Authors declare that there is no conflict of interest.
Figures

References
-
- Jencks SF, Williams MV, Coleman EA. Rehospitalizations among patients in the Medicare fee-for-service program. New England Journal of Medicine 2009;360:1418–28. - PubMed
-
- Zuckerman RB, Joynt Maddox KE, Sheingold SH, Chen LM, Epstein AM. Effect of a hospital-wide measure of the Readmissions Reduction Program. The New England Journal of Medicine 2017;377:1551–8. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

