The Importance of the Microbiome in Critically Ill Patients: Role of Nutrition
- PMID: 31817895
- PMCID: PMC6950228
- DOI: 10.3390/nu11123002
The Importance of the Microbiome in Critically Ill Patients: Role of Nutrition
Abstract
Critically ill patients have an alteration in the microbiome in which it becomes a disease-promoting pathobiome. It is characterized by lower bacterial diversity, loss of commensal phyla, like Firmicutes and Bacteroidetes, and a domination of pathogens belonging to the Proteobacteria phylum. Although these alterations are multicausal, many of the treatments administered to these patients, like antibiotics, play a significant role. Critically ill patients also have a hyperpermeable gut barrier and dysregulation of the inflammatory response that favor the development of the pathobiome, translocation of pathogens, and facilitate the emergence of sepsis. In order to restore the homeostasis of the microbiome, several nutritional strategies have been evaluated with the aim to improve the management of critically ill patients. Importantly, enteral nutrition has proven to be more efficient in promoting the homeostasis of the gut microbiome compared to parenteral nutrition. Several nutritional therapies, including prebiotics, probiotics, synbiotics, and fecal microbiota transplantation, are currently being used, showing variable results, possibly due to the unevenness of clinical trial conditions and the fact that the beneficial effects of probiotics are specific to particular species or even strains. Thus, it is of great importance to better understand the mechanisms by which nutrition and supplement therapies can heal the microbiome in critically ill patients in order to finally implement them in clinical practice with optimal safety and efficacy.
Keywords: critically ill patient; fecal microbiota transplantation; microbiome; nutrition; prebiotics; probiotics; synbiotics.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

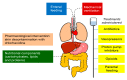
References
-
- Robertson L.C., Al-Haddad M. Recognizing the critically ill patient. Anaesth. Intensive Care Med. 2013;14:11–14. doi: 10.1016/j.mpaic.2012.11.010. - DOI

