Effects of metformin administration on endocrine-metabolic parameters, visceral adiposity and cardiovascular risk factors in children with obesity and risk markers for metabolic syndrome: A pilot study
- PMID: 31821361
- PMCID: PMC6903728
- DOI: 10.1371/journal.pone.0226303
Effects of metformin administration on endocrine-metabolic parameters, visceral adiposity and cardiovascular risk factors in children with obesity and risk markers for metabolic syndrome: A pilot study
Abstract
Background: Metformin treatment (1000-2000 mg/day) over 6 months in pubertal children and/or adolescents with obesity and hyperinsulinism is associated with a reduction in body mass index (BMI) and the insulin resistance index (HOMA-IR). We aimed to ascertain if long-term treatment (24 months) with lower doses of metformin (850 mg/day) normalizes the endocrine-metabolic abnormalities, improves body composition, and reduces the carotid intima-media thickness (cIMT) in pre-puberal and early pubertal children with obesity.
Methods: A pilot double-blind, placebo-controlled trial was conducted on 18 pre-puberal and early pubertal (Tanner stage I-II) children with obesity and risk markers for metabolic syndrome. Patients were randomly assigned (1:1) to receive metformin (850 mg/day) or placebo for 24 months. Clinical, biochemical (insulin, lipids, leptin, and high-sensitivity C-reactive protein [hsCRP]), and imaging (body composition [dual-energy X-ray absorptiometry and magnetic resonance imaging]) parameters as well as cIMT (ultrasonography) were assessed at baseline and at 6, 12, and 24 months.
Results: The 12-month treatment tend to cause a reduction in weight standard deviation scores (SDS), BMI-SDS, leptin, leptin-to-high-molecular-weight (HMW) adiponectin ratio, hsCRP, cIMT, fat mass, and liver fat in metformin-treated children compared with placebo. The effect of metformin on the reduction of BMI-SDS, leptin, leptin-to-HMW adiponectin ratio, hsCRP, and liver fat seemed to be maintained after completing the 24 months of treatment. No changes in insulin sensitivity (HOMA-IR) or adverse effects were detected.
Conclusion: In this pilot study, metformin treatment in pre-puberal and early pubertal children with obesity seemed to improve body composition and inflammation markers. Our data encourage the development of future fully powered trials using 850 mg/day metformin in young children, highlighting its excellent tolerance and potential long-term benefits.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures

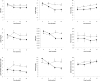

References
-
- Serra-Majem L, Aranceta Bartrina J, Perez-Rodrigo C, Ribas-Barba L, Delgado-Rubio A. Prevalence and deteminants of obesity in Spanish children and young people. The British journal of nutrition. 2006, 96 Suppl 1:S67–72. - PubMed
-
- Weihrauch-Bluher S, Schwarz P, Klusmann JH. Childhood obesity: increased risk for cardiometabolic disease and cancer in adulthood. Metabolism: clinical and experimental. 2019; 92:147–152. - PubMed
-
- August GP, Caprio S, Fennoy I, Freemark M, Kaufman FR, Lustig RH, et al. Prevention and treatment of pediatric obesity: an endocrine society clinical practice guideline based on expert opinion. The Journal of clinical endocrinology and metabolism. 2008, 93:4576–4599. 10.1210/jc.2007-2458 - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

