A Systems Pharmacology Model for Drug Delivery to Solid Tumors by Antibody-Drug Conjugates: Implications for Bystander Effects
- PMID: 31828446
- PMCID: PMC7098807
- DOI: 10.1208/s12248-019-0390-2
A Systems Pharmacology Model for Drug Delivery to Solid Tumors by Antibody-Drug Conjugates: Implications for Bystander Effects
Abstract
Antibody-drug conjugates (ADCs) are cancer drugs composed of a humanized antibody linked to a cytotoxic payload, allowing preferential release of payload in cancer cells expressing the antibody-targeted antigen. Here, a systems pharmacology model is used to simulate ADC transport from blood to tumor tissue and ADC uptake by tumor cells. The model includes effects of spatial gradients in drug concentration in a three-dimensional network of tumor blood vessels with realistic geometry and accounts for diffusion of ADC in the tumor extracellular space, binding to antigen, internalization, intracellular processing, and payload efflux from cells. Cells that process an internalized ADC-antigen complex may release payload that can be taken up by other "bystander" cells. Such bystander effects are included in the model. The model is used to simulate conditions in previous experiments, showing good agreement with experimental results. Simulations are used to analyze the relationship of bystander effects to payload properties and single-dose administrations. The model indicates that exposure of payload to cells distant from vessels is sensitive to the free payload diffusivity in the extracellular space. When antigen expression is heterogeneous, the model indicates that the amount of payload accumulating in non-antigen-expressing cells increases linearly with dose but depends only weakly on the percentage of antigen-expressing cells. The model provides an integrated mechanistic framework for understanding the effects of spatial gradients on drug distribution using ADCs and for designing ADCs to achieve more effective payload distribution in solid tumors, thereby increasing the therapeutic index of the ADC.
Keywords: capillaries; diffusion; drug transport; mathematical model; vascular permeability.
Figures



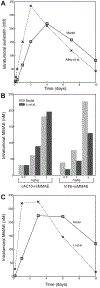



References
-
- Sanderson RJ, Hering MA, James SF, Sun MMC, Doronina SO, Siadak AW, et al. In vivo Drug-Linker Stability of an Anti-CD30 Dipeptide-Linked Auristatin Immunoconjugate. Clinical Cancer Research. 2005;11:843–52. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources

