US Trends in Hospitalizations for Dialysis-Requiring Acute Kidney Injury in People With Versus Without Diabetes
- PMID: 31843236
- PMCID: PMC11000252
- DOI: 10.1053/j.ajkd.2019.09.012
US Trends in Hospitalizations for Dialysis-Requiring Acute Kidney Injury in People With Versus Without Diabetes
Abstract
Rationale & objective: Dialysis-requiring acute kidney injury (AKI-D) has increased substantially in the United States. We examined trends in and comorbid conditions associated with hospitalizations and in-hospital mortality in the setting of AKI-D among people with versus without diabetes.
Study design: Cross-sectional study.
Setting & participants: Nationally representative data from the National Inpatient Sample and National Health Interview Survey were used to generate 16 cross-sectional samples of US adults (aged ≥18 years) between 2000 and 2015.
Exposure: Diabetes, defined using International Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM) diagnosis codes.
Outcome: AKI-D, defined using ICD-9-CM diagnosis and procedure codes.
Analytical approach: Annual age-standardized rates of AKI-D and AKI-D mortality were calculated for adults with and without diabetes, by age and sex. Data were weighted to be representative of the US noninstitutionalized population. Trends were assessed using join point regression with annual percent change (Δ/y) reported.
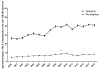
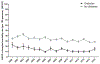
Results: In adults with diabetes, AKI-D increased between 2000 and 2015 (from 26.4 to 41.1 per 100,000 persons; Δ/y, 3.3%; P < 0.001), with relative increases greater in younger versus older adults. In adults without diabetes, AKI-D increased between 2000 and 2009 (from 4.8 to 8.7; Δ/y, 6.5%; P < 0.001) and then plateaued. AKI-D mortality significantly declined in people with and without diabetes. In adults with and without diabetes, the proportion of AKI-D hospitalizations with liver, rheumatic, and kidney disease comorbid conditions increased between 2000 and 2015, while the proportion of most cardiovascular comorbid conditions decreased.
Limitations: Lack of laboratory data to corroborate AKI diagnosis; National Inpatient Sample data are hospital-level rather than person-level data; no data for type of diabetes; residual unmeasured confounding.
Conclusions: Hospitalization rates for AKI-D have increased considerably while mortality has decreased in adults with and without diabetes. Hospitalization rates for AKI-D remain substantially higher in adults with diabetes. Greater AKI risk-factor mitigation is needed, especially in young adults with diabetes.
Keywords: AKI risk factor; AKI stage 3; Acute kidney injury (AKI); age; comorbidity; diabetes mellitus (DM); diabetes-related complications; dialysis-requiring AKI (AKI-D); epidemiology; hospitalization; in-hospital mortality; mortality; renal failure; secular trend.
Copyright © 2019 National Kidney Foundation, Inc. Published by Elsevier Inc. All rights reserved.
Conflict of interest statement
Figures
References
-
- Lameire N, Biesen WV, Vanholder R. Acute kidney injury. Lancet. 2008;372(9653):1863–1865. - PubMed
-
- Moore BJ,Torio CM. Acute Renal Failure Hospitalizations, 2005-2014: Statistical Brief #231. Rockville, MD: Healthcare Cost and Utilization Project (HCUP) Statistical Briefs; 2006.
-
- Liangos O, Wald R, O’Bell JW, Price L, Pereira BJ, Jaber BL. Epidemiology and outcomes of acute renal failure in hospitalized patients: a national survey. Clin J Am Soc Nephrol. 2006;1(1):43–51. - PubMed
-
- Kerr M, Bedford M, Matthews B, O’Donoghue D. The economic impact of acute kidney injury in England. Nephrol Dial Transplant. 2014;29(7):1362–1368. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

