Diagnosis Across the Spectrum of Progressive Supranuclear Palsy and Corticobasal Syndrome
- PMID: 31860007
- PMCID: PMC6990759
- DOI: 10.1001/jamaneurol.2019.4347
Diagnosis Across the Spectrum of Progressive Supranuclear Palsy and Corticobasal Syndrome
Abstract
Importance: Atypical parkinsonian syndromes (APS), including progressive supranuclear palsy (PSP), corticobasal syndrome (CBS), and multiple system atrophy (MSA), may be difficult to distinguish in early stages and are often misdiagnosed as Parkinson disease (PD). The diagnostic criteria for PSP have been updated to encompass a range of clinical subtypes but have not been prospectively studied.
Objective: To define the distinguishing features of PSP and CBS subtypes and to assess their usefulness in facilitating early diagnosis and separation from PD.
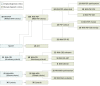
Design, setting, participants: This cohort study recruited patients with APS and PD from movement disorder clinics across the United Kingdom from September 1, 2015, through December 1, 2018. Patients with APS were stratified into the following groups: those with Richardson syndrome (PSP-RS), PSP-subcortical (including PSP-parkinsonism and progressive gait freezing subtypes), PSP-cortical (including PSP-frontal and PSP-CBS overlap subtypes), MSA-parkinsonism, MSA-cerebellar, CBS-Alzheimer disease (CBS-AD), and CBS-non-AD. Data were analyzed from February 1, through May 1, 2019.
Main outcomes and measures: Baseline group comparisons used (1) clinical trajectory; (2) cognitive screening scales; (3) serum neurofilament light chain (NF-L) levels; (4) TRIM11, ApoE, and MAPT genotypes; and (5) volumetric magnetic resonance imaging measures.
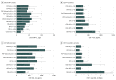
Results: A total of 222 patients with APS (101 with PSP, 55 with MSA, 40 with CBS, and 26 indeterminate) were recruited (129 [58.1%] male; mean [SD] age at recruitment, 68.3 [8.7] years). Age-matched control participants (n = 76) and patients with PD (n = 1967) were included for comparison. Concordance between the antemortem clinical and pathologic diagnoses was achieved in 12 of 13 patients with PSP and CBS (92.3%) undergoing postmortem evaluation. Applying the Movement Disorder Society PSP diagnostic criteria almost doubled the number of patients diagnosed with PSP from 58 to 101. Forty-nine of 101 patients with reclassified PSP (48.5%) did not have the classic PSP-RS subtype. Patients in the PSP-subcortical group had a longer diagnostic latency and a more benign clinical trajectory than those in PSP-RS and PSP-cortical groups. The PSP-subcortical group was distinguished from PSP-cortical and PSP-RS groups by cortical volumetric magnetic resonance imaging measures (area under the curve [AUC], 0.84-0.89), cognitive profile (AUC, 0.80-0.83), serum NF-L level (AUC, 0.75-0.83), and TRIM11 rs564309 genotype. Midbrain atrophy was a common feature of all PSP groups. Eight of 17 patients with CBS (47.1%) undergoing cerebrospinal fluid analysis were identified as having the CBS-AD subtype. Patients in the CBS-AD group had a longer diagnostic latency, relatively benign clinical trajectory, greater cognitive impairment, and higher APOE-ε4 allele frequency than those in the CBS-non-AD group (AUC, 0.80-0.87; P < .05). Serum NF-L levels distinguished PD from all PSP and CBS cases combined (AUC, 0.80; P < .05).
Conclusions and relevance: These findings suggest that studies focusing on the PSP-RS subtype are likely to miss a large number of patients with underlying PSP tau pathology. Analysis of cerebrospinal fluid defined a distinct CBS-AD subtype. The PSP and CBS subtypes have distinct characteristics that may enhance their early diagnosis.
Conflict of interest statement
Figures

References
Publication types
MeSH terms
Grants and funding
- MR/S000992/1/MRC_/Medical Research Council/United Kingdom
- G1000691/MRC_/Medical Research Council/United Kingdom
- 103838/WT_/Wellcome Trust/United Kingdom
- 548211/MRC_/Medical Research Council/United Kingdom
- G1001253/MRC_/Medical Research Council/United Kingdom
- R605/0717/DMT_/The Dunhill Medical Trust/United Kingdom
- G108/638/MRC_/Medical Research Council/United Kingdom
- MR/L022656/1/MRC_/Medical Research Council/United Kingdom
- MR/M008525/1/MRC_/Medical Research Council/United Kingdom
- MR/S01165X/1/MRC_/Medical Research Council/United Kingdom
- MR/J009482/1/MRC_/Medical Research Council/United Kingdom
- J-0901/PUK_/Parkinson's UK/United Kingdom
- G0802760/MRC_/Medical Research Council/United Kingdom
- MR/M023664/1/MRC_/Medical Research Council/United Kingdom
- MR/L010305/1/MRC_/Medical Research Council/United Kingdom
- J-1101/PUK_/Parkinson's UK/United Kingdom
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

