Activity Performance, Participation, and Quality of Life Among Adults in the Chronic Stage After Acquired Brain Injury-The Feasibility of an Occupation-Based Telerehabilitation Intervention
- PMID: 31866924
- PMCID: PMC6908485
- DOI: 10.3389/fneur.2019.01247
Activity Performance, Participation, and Quality of Life Among Adults in the Chronic Stage After Acquired Brain Injury-The Feasibility of an Occupation-Based Telerehabilitation Intervention
Abstract
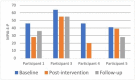
Objective: Acquired brain injury (ABI) is a leading cause of long-term disability. This calls for effective and accessible interventions to support participation in the community over time. One promising avenue to answer this need is telerehabilitation. Prior to conducting a larger trial, the main objective of this pilot study is to explore the feasibility, acceptability, and preliminary efficacy of a metacognitive occupation-based intervention in a telerehabilitation format with adults and older adults in the chronic phase after ABI. Methods: Five community dwelling participants (ages 65-72), 6-10 months post-ABI, with scores 2-4 on the modified Rankin scale and without dementia, completed the teleintervention. The intervention included ~10 weekly videoconferencing sessions administered by an occupational therapist using the Cognitive Orientation to Daily Occupational Performance approach. Each participant defined five functional goals and three were trained and two were not trained during the intervention. Evaluations were conducted at pre, post, and 3-month follow-up. The primary outcome measures included activity performance (The Canadian Occupational Performance Measure; COPM), participation (the Mayo-Portland Adaptability Inventory-4 Participation Index; MPAI-4-P), and quality of life (QoL) (stroke impact scale; SIS). Other measures included a feedback interview, satisfaction questionnaire, field notes, and a treatment fidelity checklist. Results: The teleintervention was found to be feasible and the participants expressed a high degree of satisfaction with the intervention and the technology use. A Wilcoxon Signed-Ranks test indicated statistically significant improvements post intervention in COPM performance (z = -2.023, p = 0.043) and satisfaction (z = -2.023, p = 0.043) ratings. Additionally, clinically significant improvements (≥2 points) in both performance and satisfaction with performance were found for each participant in at least three of their five defined functional goals. Trends toward significant improvement were found in MPAI-4-P ratings post intervention (z = -1.826, p = 0.068). Furthermore, clinically significant improvements (≥15 points) post intervention were found for each participant in some subscales of the SIS. Results were partially maintained at 3-month follow-up. Conclusions: This pilot study demonstrated the feasibility of a metacognitive occupation-based telerehabilitation intervention and its potential benefits in activity performance, participation, and QoL for older adults coping with long-term disability following ABI. Clinical Trial Registration: www.ClinicalTrials.gov, identifier: NCT03048708.
Keywords: activity performance; chronic acquired brain injury; cognitive orientation to daily occupational performance approach; metacognitive approach; neurorehabilitation; occupational therapy; participation; telerehabilitation.
Copyright © 2019 Beit Yosef, Jacobs, Shenkar, Shames, Schwartz, Doryon, Naveh, Khalailh, Berrous and Gilboa.
Figures



References
-
- Ciuffreda KJ, Kapoor N. Acquired brain injury. In: Taub MB, Bartuccio M, Maino DM, editors. Visual Diagnosis and Care of the Patient with Special Needs. Philadelphia, PA: Wolters Kluwer Health; Lippincott Williams and Wilkins; (2012). p. 95–100.
-
- Lannoo E, Brusselmans W, Eynde LV, Van Laere M, Stevens J. Epidemiology of acquired brain injury (ABI) in adults: prevalence of long-term disabilities and the resulting needs for ongoing care in the region of Flanders, Belgium. Brain Inj. (2004) 18:203–11. 10.1080/02699050310001596905 - DOI - PubMed
Associated data
LinkOut - more resources
Full Text Sources
Medical

