Hemocompatibility and safety of the Carmat Total Artifical Heart hybrid membrane
- PMID: 31867454
- PMCID: PMC6906674
- DOI: 10.1016/j.heliyon.2019.e02914
Hemocompatibility and safety of the Carmat Total Artifical Heart hybrid membrane
Abstract
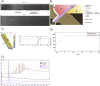
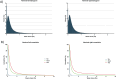
The Carmat bioprosthetic total artificial heart (C-TAH) is a biventricular pump developed to minimize drawbacks of current mechanical assist devices and improve quality of life during support. This study aims to evaluate the safety of the hybrid membrane, which plays a pivotal role in this artificial heart. We investigated in particular its blood-contacting surface layer of bovine pericardial tissue, in terms of mechanical aging, risks of calcification, and impact of the hemodynamics shear stress inside the ventricles on blood components. Hybrid membranes were aged in a custom-designed endurance bench. Mechanical, physical and chemical properties were not significantly modified from 9 months up to 4 years of aging using a simulating process. Exploration of erosion areas did not show no risk of oil diffusion through the membrane. Blood contacting materials in the ventricular cavities were subcutaneously implanted in Wistar rats for 30 days as a model for calcification and demonstrated that the in-house anti-calcification pretreatment with Formaldehyde-Ethanol-Tween 80 was able to significantly reduce the calcium concentration from 132 μg/mg to 4.42 μg/mg (p < 0.001). Hemodynamic simulations with a computational model were used to reproduce shear stress in left and right ventricles and no significant stress was able to trigger hemolysis, platelet activation nor degradation of the von Willebrand factor multimers. Moreover, explanted hybrid membranes from patients included in the feasibility clinical study were analyzed confirming preclinical results with the absence of significant membrane calcification. At last, blood plasma bank analysis from the four patients implanted with C-TAH during the feasibility study showed no residual glutaraldehyde increase in plasma and confirmed hemodynamic simulation-based results with the absence of hemolysis and platelet activation associated with normal levels of plasma free hemoglobin and platelet microparticles after C-TAH implantation. These results on mechanical aging, calcification model and hemodynamic simulations predicted the safety of the hybrid membrane used in the C-TAH, and were confirmed in the feasibility study.
Keywords: Bioengineering; Biomedical engineering; Biophysics; Bioprosthetic; Cardiology; Carmat; Haematology; Hemocompatibility; Total artificial heart.
© 2019 Published by Elsevier Ltd.
Figures




References
-
- Rossano J.W., Dipchand A.I., Edwards L.B., Goldfarb S., Kucheryavaya A.Y., Levvey B.J., RN, Lund L.H., Meiser B., Yusen R.D., Stehlik J. The registry of the international society for heart and lung transplantation: nineteenth pediatric heart transplantation report—2016; focus theme: primary diagnostic indications for transplant. J. Heart Lung Transplant. 2016;35:1185–1195. - PubMed
-
- Hunt S.A., Rose E.A. The REMATCH trial: long-term use of a left ventricular assist device for end-stage heart failure. Rev. Port. Cardiol. 2001;20:1279–1280. - PubMed
-
- Kirklin J.K., Pagani F.D., Kormos R.L., Stevenson L.W., Blume E.D., Myers S.L., Miller M.A., Baldwin J.T., Young J.B., Naftel D.C. Eighth annual INTERMACS report: special focus on framing the impact of adverse events. J. Heart Lung Transplant. 2017;36:1080–1086. - PubMed
-
- Carpentier A., Latrémouille C., Cholley B., Smadja D.M., Roussel J.C., Boissier E., Trochu J.N., Gueffet J.P., Treillot M., Bizouarn P., Méléard D., Boughenou M.F., Ponzio O., Grimmé M., Capel A., Jansen P., Hagège A., Desnos M., Fabiani J.N., Duveau D. First clinical use of a bioprosthetic total artificial heart: report of two cases. Lancet. 2015;386:1556–1563. - PubMed
-
- Jansen P., van Oeveren W., Capel A., Carpentier A. In vitro haemocompatibility of a novel bioprosthetic total artificial heart. Eur. J. Cardiothorac. Surg. 2012;41 - PubMed
LinkOut - more resources
Full Text Sources

