Great variability in donor heart acceptance practices across the United States
- PMID: 31883229
- PMCID: PMC7261633
- DOI: 10.1111/ajt.15760
Great variability in donor heart acceptance practices across the United States
Abstract
Disparities in organ acceptance practices exacerbate donor heart nonuse and lead to increased waiting times and mortality for heart transplant candidates. We studied disparities in donor heart acceptance among US transplant centers and their relations to posttransplant outcomes. Candidate, potential transplant recipient match run, and deceased donor data were obtained from the United Network for Organ Sharing. We analyzed donor, candidate, and transplant center characteristics with respect to organ acceptance, offer acceptance, number of offers before acceptance (organ sequence number), and association with posttransplant mortality. A total of 693 420 donor heart offers made between April 2007 and December 2015 were included. We identified great variability in donor heart acceptance practices among US heart transplant centers. We identified donor and recipient characteristics that were strongly associated with heart organ and offer acceptance, and organ sequence number, and identified inconsistencies among centers with respect to how these characteristics influenced acceptance decisions. Finally, we identified characteristics that were highly predictive of donor heart nonuse and were not associated with increased recipient mortality, which may guide future efforts aimed at increasing use of available hearts for transplantation.
Keywords: clinical research/practice; donors and donation; heart transplantation/cardiology; organ acceptance; organ procurement and allocation.
© 2019 The American Society of Transplantation and the American Society of Transplant Surgeons.
Conflict of interest statement
DISCLOSURE
The authors of this manuscript have no conflicts of interest to disclose as described by the
Figures



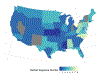



Comment in
-
True, true, and possibly unrelated: Variability in donor heart acceptance practices across the United States.Am J Transplant. 2020 Jun;20(6):1477-1479. doi: 10.1111/ajt.15855. Epub 2020 May 16. Am J Transplant. 2020. PMID: 32185879 No abstract available.
References
-
- Colvin M, Smith JM, Hadley N et al. OPTN/SRTR 2017 Annual Data Report: Heart. Am J Transplant 2019;19 Suppl 2:323–403. - PubMed
-
- Kobashigawa J, Khush K, Colvin M et al. Report From the American Society of Transplantation Conference on Donor Heart Selection in Adult Cardiac Transplantation in the United States. Am J Transplant 2017;17(10):2559–2566. - PubMed
-
- Aliabadi-Zuckermann AZ, Gokler J, Kaider A et al. Donor heart selection and outcomes: An analysis of over 2,000 cases. J Heart Lung Transplant 2018. - PubMed
-
- Chen C, Atluri P. Expanded donor selection criteria can increase organ utilization. J Heart Lung Transplant 2018;37(3):427. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

