Comparison of the Effects of Target-Controlled Infusion of Propofol and Sevoflurane as Maintenance of Anesthesia on Hemodynamic Profile in Kidney Transplantation
- PMID: 31885551
- PMCID: PMC6925739
- DOI: 10.1155/2019/5629371
Comparison of the Effects of Target-Controlled Infusion of Propofol and Sevoflurane as Maintenance of Anesthesia on Hemodynamic Profile in Kidney Transplantation
Abstract
Background: Target-controlled infusion (TCI) propofol and sevoflurane are common agents for general anesthesia, including for kidney transplantation procedure. This study compared the effect of TCI propofol and sevoflurane on intraoperative hemodynamic profile in kidney transplant patients.
Methods: A single-blinded prospective study was performed in 46 kidney transplant recipients who were randomized into receiving TCI propofol or sevoflurane as anesthetics maintenance. Hemodynamic parameters such as mean arterial pressure (MAP), cardiac index (CI), stroke volume index (SVI), and systemic vascular resistance index (SVRI) were measured at baseline before induction, postintubation, first surgical incision, every 15 minutes after the first incision, reperfusion, and 15 minutes after reperfusion. Data were analyzed using unpaired t-test, paired t-test, and general linear model.
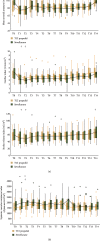
Results: Intraoperative MAP, CI, SVI, and SVRI changes were similar in both groups (p = 0.480, 0.216, 0.086, and 0.054). In comparison to the baseline value, TCI propofol and sevoflurane groups showed significant reductions of MAP at postintubation (p=0.010; p < 0.001) and during the first surgical incision (p=0.009; p < 0.001); significant reduction of CI at postintubation (p=0.003; p < 0.001) and during the first surgical incision (p < 0.001; p < 0.001); significant reduction of SVI at postintubation (p=0.013; p=0.008), during the first surgical incision (p=0.008; p=0.003), and 15 minutes after reperfusion (p=0.010; p=0.005); and significant increasing of SVRI during the first surgical incision (p=0.007; p=0.005). The TCI propofol group showed significantly lower SVRI compared to the sevoflurane group postintubation (p=0.029) and during the first surgical incision (p=0.026).
Conclusion: Intraoperative hemodynamic profile was similar between the TCI propofol and sevoflurane group during kidney transplant surgery. The TCI propofol group had higher CI and SVI but showed significantly lower SVRI as compared to the sevoflurane group. The incidence of postanesthesia agitation, postoperative outcome, and complication were not significantly different between the two groups.
Copyright © 2019 Dita Aditianingsih et al.
Conflict of interest statement
The authors declare that there are no conflicts of interest regarding the publication of this paper.
Figures

Similar articles
-
Propofol TCI or sevoflurane anesthesia without muscle relaxant for thoracoscopic thymectomy in myasthenia gravis patients: a prospective, observational study.BMC Anesthesiol. 2023 Oct 21;23(1):349. doi: 10.1186/s12871-023-02296-6. BMC Anesthesiol. 2023. PMID: 37865733 Free PMC article.
-
Comparative randomized study of propofol target-controlled infusion versus sevoflurane anesthesia for third molar extraction.J Dent Anesth Pain Med. 2018 Jun;18(3):169-175. doi: 10.17245/jdapm.2018.18.3.169. Epub 2018 Jun 29. J Dent Anesth Pain Med. 2018. PMID: 29984321 Free PMC article.
-
[Comparison of target controlled propofol infusion and sevoflurane inhalational anesthesia in laparoscopic cholecystectomy].Nan Fang Yi Ke Da Xue Xue Bao. 2007 Aug;27(8):1280-1, 1284. Nan Fang Yi Ke Da Xue Xue Bao. 2007. PMID: 17715049 Clinical Trial. Chinese.
-
A comparison of propofol target controlled infusion-based and sevoflurane-based anesthesia in adults undergoing elective anterior cervical discectomy and fusion.Kaohsiung J Med Sci. 2015 Mar;31(3):150-5. doi: 10.1016/j.kjms.2014.12.002. Epub 2015 Jan 20. Kaohsiung J Med Sci. 2015. PMID: 25744238 Free PMC article.
-
Effects of Sevoflurane and Propofol During Mechanical Ventilation: A Meta-analysis of Randomized Controlled Trials.J Perianesth Nurs. 2025 Apr 8:S1089-9472(24)00562-8. doi: 10.1016/j.jopan.2024.12.001. Online ahead of print. J Perianesth Nurs. 2025. PMID: 40202471 Review.
Cited by
-
Monitoring the effects of automated gas control of sevoflurane versus target-guided propofol infusion on hemodynamics of liver patients during liver resection. A randomized controlled trial.J Anaesthesiol Clin Pharmacol. 2023 Jan-Mar;39(1):74-83. doi: 10.4103/joacp.joacp_168_21. Epub 2022 Jan 10. J Anaesthesiol Clin Pharmacol. 2023. PMID: 37250255 Free PMC article.
-
Application of Propofol Target-Controlled Infusion for Optimized Hemodynamic Status in ESRD Patients Receiving Arteriovenous Access Surgery: A Randomized Controlled Trial.Medicina (Kaunas). 2022 Sep 1;58(9):1203. doi: 10.3390/medicina58091203. Medicina (Kaunas). 2022. PMID: 36143879 Free PMC article. Clinical Trial.
-
Inhaled Anesthetics: Environmental Role, Occupational Risk, and Clinical Use.J Clin Med. 2021 Mar 22;10(6):1306. doi: 10.3390/jcm10061306. J Clin Med. 2021. PMID: 33810063 Free PMC article. Review.
References
-
- Kashkouli A., Moradi A., Torabian S., Amir-Zargar M., Gholyaf M. Comparison of safety and efficacy of general and spinal anesthesia in kidney transplantation: evaluation of the peri-operative outcome. Saudi Journal of Kidney Diseases and Transplantation. 2015;26(3):p. 447. doi: 10.4103/1319-2442.157300. - DOI - PubMed
-
- Cingi E., Beebe D. S., Harmon J. V., Jr., Belani K. Anesthesia and Perioperative Care for Organ Transplantation. New York, NY, USA: Springer Nature; 2016. Preoperative recipient evaluation and preparation (kidney) pp. 275–280. - DOI
LinkOut - more resources
Full Text Sources

