Clinicopathological Characteristics and Breast Cancer-Specific Survival of Patients With Single Hormone Receptor-Positive Breast Cancer
- PMID: 31899528
- PMCID: PMC6991239
- DOI: 10.1001/jamanetworkopen.2019.18160
Clinicopathological Characteristics and Breast Cancer-Specific Survival of Patients With Single Hormone Receptor-Positive Breast Cancer
Abstract
Importance: Steroid hormone receptors, including estrogen receptor (ER) and progesterone receptor (PR), are crucial biomarkers in breast cancer (BC). However, limited data are available regarding single hormone receptor-positive (ER-positive/PR-negative and ER-negative/PR-positive) subtypes, rendering treatment decision and survival forecast difficult in patients with these BC subtypes.
Objective: To investigate the clinicopathological characteristics and BC-specific survival (BCSS) of patients with single hormone receptor-positive BC.
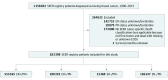
Design, setting, and participants: In this cohort study, data on patients diagnosed with BC between 1990 and 2015 were retrieved from the Surveillance, Epidemiology, and End Results database (N = 1 158 032). Patients lacking information on ER status, PR status, or BCSS were excluded (n = 334 633). Comparisons were performed between single hormone receptor-positive BC and double hormone receptor-positive/double hormone receptor-negative BC. The dates of analysis were September 1, 2018, to June 31, 2019.
Main outcomes and measures: The BCSS of patients with single hormone receptor-positive BC.
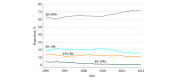
Results: This cohort study included 823 399 patients with BC (818 002 women and 5397 men). The median (range) age at diagnosis was 60 (8-108) years, and the median (range) follow-up duration was 71 (0-311) months. The percentages of ER-positive/PR-positive, ER-positive/PR-negative, ER-negative/PR-positive, and ER-negative/PR-negative cases were 67.2%, 12.2%, 1.6%, and 19.0%, respectively. Single hormone receptor-positive subtypes showed distinct clinical characteristics compared with double hormone receptor-positive/double hormone receptor-negative subtypes. Multivariable Cox proportional hazards regression analysis showed that patients with ER-positive/PR-negative (hazard ratio [HR], 1.36; 95% CI, 1.34-1.38) and ER-negative/PR-positive (HR, 1.61; 95% CI, 1.55-1.67) tumors had worse BCSS than patients with the ER-positive/PR-positive subtype. In contrast, patients with ER-positive/PR-negative (HR, 1.27; 95% CI, 1.24-1.29) and ER-negative/PR-positive (HR, 1.07; 95% CI, 1.03-1.11) tumors had better BCSS than patients with the ER-negative/PR-negative subtype. The BCSS was statistically significantly worse in patients with ER-negative/PR-positive tumors than in patients with ER-positive/PR-negative tumors (HR, 1.18; 95% CI, 1.14-1.23).
Conclusions and relevance: In this cohort study, statistically significant distinctions between survival rates of patients with single hormone receptor-positive BC vs double hormone receptor-positive/double hormone receptor-negative BC were observed. Different strategies may be required for patients with single hormone receptor-positive tumors to ensure optimal treatment and maximum benefits from therapies.
Conflict of interest statement
Figures

Comment in
-
Single Hormone Receptor-Positive Breast Cancer-Signal or Noise?JAMA Netw Open. 2020 Jan 3;3(1):e1918176. doi: 10.1001/jamanetworkopen.2019.18176. JAMA Netw Open. 2020. PMID: 31899524 No abstract available.
References
-
- Bardou VJ, Arpino G, Elledge RM, Osborne CK, Clark GM. Progesterone receptor status significantly improves outcome prediction over estrogen receptor status alone for adjuvant endocrine therapy in two large breast cancer databases. J Clin Oncol. 2003;21(10):-. doi:10.1200/JCO.2003.09.099 - DOI - PubMed
-
- Hammond ME, Hayes DF, Dowsett M, et al. . American Society of Clinical Oncology/College of American Pathologists guideline recommendations for immunohistochemical testing of estrogen and progesterone receptors in breast cancer. J Clin Oncol. 2010;28(16):2784-2795. doi:10.1200/JCO.2009.25.6529 - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials

