What Factors are Associated with Revision or Worse Patient-reported Outcome after Reverse Shoulder Arthroplasty for Cuff-tear Arthropathy? A Study from the Danish Shoulder Arthroplasty Registry
- PMID: 31899740
- PMCID: PMC7170693
- DOI: 10.1097/CORR.0000000000001114
What Factors are Associated with Revision or Worse Patient-reported Outcome after Reverse Shoulder Arthroplasty for Cuff-tear Arthropathy? A Study from the Danish Shoulder Arthroplasty Registry
Abstract
Background: Reverse shoulder arthroplasty has been proven to improve function in shoulders with cuff-tear arthropathy, but existing studies are primarily single-center studies with a small number of patients, which limits their ability to identify patients who have an increased risk of revision or a worse functional outcome.
Questions/purposes: (1) What is the estimated 10-year cumulative revision rate after reverse shoulder arthroplasty for cuff-tear arthropathy, and what factors are associated with the risk of revision? (2) What is the patient-reported outcome 1 year after surgery, and what factors are associated with a worse patient-reported outcome?
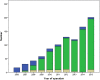
Methods: We included all patients treated with reverse shoulder arthroplasty for cuff-tear arthropathy reported in the Danish Shoulder Arthroplasty Registry from 2006 to 2015. During the study period, the completeness of reporting was 93% for both primary and revision arthroplasties. Estimated revision rates were illustrated using the Kaplan-Meier method, and hazard ratios were calculated using a Cox regression model. Patient-reported outcome was measured with a postal survey at 12 months (range 10-14 months) postoperatively using the Western Ontario Osteoarthritis of the Shoulder (WOOS) index. The WOOS is a patient-administered questionnaire that measures the quality of life of patients with glenohumeral osteoarthritis. A visual analog scale that ranges from 0 to 100 is used for each question. There are 19 questions, giving a total score ranging from 0 to 1900, with 1900 being the worst. For simplicity of presentation, raw scores were converted to a percentage of the maximum score, with 100 being the best. There is no defined minimal clinically important difference of the WOOS, but the Danish Shoulder arthroplasty registry has for many years regarded an arbitrary difference of 10 or above as being clinically relevant. The rate of response to the WOOS was 71%.
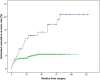
Results: The estimated 10-year cumulative revision rate was 8.5% (95% confidence interval, 5.7%-11.3%) with differences between the arthroplasty model (21.0%; 95% CI, 11.8% to 30.8% for the Delta Mark III and 5.5%; 95% CI, 3.7% to 7.3% for the Delta Xtend) and gender (6.0%; 95% CI, 3.0% to 9.0% for women and 13.1%; 95% CI, 7.1% to 19.1% for men). After controlling for potential confounding variables including gender, previous surgery, arthroplasty model, and period of surgery, the risk of revision was higher with the Delta Mark III than with the Delta Xtend (hazard ratio 2.7; 95% CI, 1.3 to 5.4; p < 0.01) and higher in men than in women (hazard ratio 2.7; 95% CI, 1.6 to 4.7; p < 0.01). Thirty-three percent (19 of 57) of the revision arthroplasties were performed for dislocation and 32% (18 of 57) were to treat periprosthetic joint infection. After controlling for confounding variables, only previous surgery was associated with a worse WOOS score (mean difference -10.6; 95% CI, -15.2 to -5.9; p < 0.01); there were no associations between a worse score and gender, arthroplasty model, age group, or period of surgery.
Conclusions: The results from the present study can be used to inform patients about their individual risk of revision or a disappointing functional outcome. The study also demonstrates the need for proper patient selection and attention to technical details to reduce the risk of revision, especially for men. Our follow-up time was, however, short, with only an estimate of the 10-year revision rate. Future studies with a long-term follow-up duration are needed to confirm our results.
Level of evidence: Level III, therapeutic study.
Conflict of interest statement
Each author certifies that neither he, nor any member of his immediate family, has funding or commercial associations (consultancies, stock ownership, equity interest, patent/licensing arrangements, etc.) that might pose a conflict of interest in connection with the submitted article.
All ICMJE Conflict of Interest Forms for authors and
Figures


Comment in
-
CORR Insights®: What Factors are Associated with Revision or Worse Patient-reported Outcomes after Reverse Shoulder Arthroplasty for Cuff-tear Arthropathy? A Study from the Danish Shoulder Arthroplasty Registry.Clin Orthop Relat Res. 2020 May;478(5):1098-1100. doi: 10.1097/CORR.0000000000001176. Clin Orthop Relat Res. 2020. PMID: 32091428 Free PMC article. No abstract available.
References
-
- Al-Hadithy N, Domos P, Sewell MD, Pandit R. Reverse shoulder arthroplasty in 41 patients with cuff tear arthropathy with a mean follow-up period of 5 years. J Shoulder Elbow Surg. 2014;23:1662-1668. - PubMed
-
- Australian Ortopaedic Asssociation National Joint Replacement Registry. 2017. annual report. Demographics and outcome of shoulder arthroplasty. Available at: https://aoanjrr.sahmri.com/fi/annual-reports-2017. Accessed December 19, 2017.
-
- Baui DJ, Latouche A, Porcher R. Competing events influence estimated survival propability: when is Kaplan Meier analysis appropriate? Clin Orthop Relat Res. 200:229-233. - PubMed
-
- Boileau P, Watkinson D, Hatzidakis AM, Hovorka I. Neer Award 2005: the Grammont reverse shoulder prosthesis: results in cuff tear arthritis, fracture sequelae, and revision arthroplasty. J Shoulder Elbow Surg. 2006;15:527-540. - PubMed
-
- Danish Shoulder Arthroplasty Registry. 2017. annual report. Available at: https://www.sundhed.dk/content/cms/3/4703_dansk-skulderalloplastik-regis.... Accessed December 19, 2017.
MeSH terms
LinkOut - more resources
Full Text Sources

