Can we differentiate histologic subtypes of neuroendocrine tumour liver metastases at a single phase contrast-enhanced CT-correlation with Ga-68 DOTATATE PET/CT findings
- PMID: 31922897
- PMCID: PMC7055452
- DOI: 10.1259/bjr.20190735
Can we differentiate histologic subtypes of neuroendocrine tumour liver metastases at a single phase contrast-enhanced CT-correlation with Ga-68 DOTATATE PET/CT findings
Abstract
Objective: To assess the usefulness of a single-phase contrast-enhanced CT to differentiate subtypes of neuroendocrine tumour (NET) liver metastases and to evaluate the correlation between CT features and Ga-68 DOTATATE positron emission tomography/CT (PET/CT) findings.
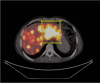
Methods: Between December 2017 and April 2019 patients with liver metastases of neuroendocrine tumours who underwent CT and Ga-68 DOTATATE PET/CT were enrolled in the study. All patients involved in the study had undergone a standardised single-phase contrast-enhanced CT. Whole body PET/CT images were obtained with a combined PET/CT scanner. All CT images were retrospectively analysed by two radiologists. Enhancement patterns of lesions were assessed. For quantitative examination; CT attenuation values of metastatic lesions, liver parenchyma and aorta were measured using a freehand ROI and tumour-to-liver ratio [T-L = (Tumour-Liver) / Liver] and tumour-to-aorta ratio [T-A = (Tumour-Aorta) / Aorta] were calculated. The lesion with the highest Ga-68 DOTATATE uptake in the liver was used for calculations. The metabolic tumour volume (MTV), maximum standardised uptake value (SUV max) and SUV mean were calculated for the target liver lesion.
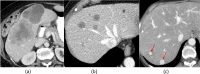
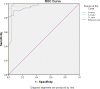
Results: A total of 137 NET liver metastases divided into in three groups: 49 (35.7%) pancreatic, 60 (44.5%) gastroenteric and 26 (18.9%) lung NET liver metastases were analysed. Gastroenteric NET metastases often showed heterogeneous enhancement which was significantly higher than in the pancreas and lung NET liver metastases (p < 0.001). 96.72% (n = 59) of the gastroenteric NET liver metastases were hypoattenuating whereas the most frequent presentation for the pancreatic group was hyperattenuation (63.26%,n = 31). The difference in enhancement patterns of the liver metastases was statistically significant (p < 0.001) with respect to the location of the primary tumour. For quantitative analysis; tumour CT values were significantly different between the groups (p < 0.001). The T-L ratio was statistically different between gastroenteric and pancreatic NET liver metastases and pancreatic and lung NET groups (p < 0.001). The T-A ratio was significantly higher in the pancreatic NET metastases (p < 0.001). SUVmax, SUVmean and MTV values, however, were not significantly different between the subgroups. There was a weak positive correlation between T-L ratio and SUV meanvalues.
Conclusion: We noticed statistically significant differences in both qualitative and quantitative CT features between histologic subgroups of neuroendocrine tumour liver metastases at a single phase contrast-enhanced CT.
Advances in knowledge: Our study will be the first in the literature which extensively focus on assessing the CT features of liver metastases of NETs at a single phase CT and Ga-68DOTATATE PET/CT. As the different histological subtypes of NET liver metastases exhibit different clinical outcomes, these features might help to identify the primary tumour to provide optimal treatment.
Figures
Similar articles
-
Liver metastases of neuroendocrine tumors: is it possible to diagnose different histologic subtypes depending on multiphasic CT features?Abdom Radiol (NY). 2019 Jun;44(6):2147-2155. doi: 10.1007/s00261-019-01963-y. Abdom Radiol (NY). 2019. PMID: 30863999
-
68 Ga DOTATATE PET/MR Imaging of Well-Differentiated Primary and Metastatic Liver Neuroendocrine Tumors : Unified Evaluation and Correlations of PET, DCE, DWI, and T2-weighted Images.Clin Nucl Med. 2025 Sep 1;50(9):e531-e542. doi: 10.1097/RLU.0000000000005994. Epub 2025 May 27. Clin Nucl Med. 2025. PMID: 40424605
-
A prospective head-to-head comparison of 68 Ga-NOTA-3P-TATE-RGD and 68 Ga-DOTATATE in patients with gastroenteropancreatic neuroendocrine tumours.Eur J Nucl Med Mol Imaging. 2022 Oct;49(12):4218-4227. doi: 10.1007/s00259-022-05852-3. Epub 2022 Jun 3. Eur J Nucl Med Mol Imaging. 2022. PMID: 35657429 Clinical Trial.
-
Cardiac neuroendocrine tumour metastases: case reports and review of the literature.Nucl Med Commun. 2016 May;37(5):461-5. doi: 10.1097/MNM.0000000000000464. Nucl Med Commun. 2016. PMID: 26671851 Review.
-
Diagnostic value of [68 Ga]Ga-DOTA-labeled-somatostatin analogue PET/MRI for detecting liver metastasis in patients with neuroendocrine tumors: a systematic review and meta-analysis.Eur Radiol. 2022 Jul;32(7):4628-4637. doi: 10.1007/s00330-021-08527-z. Epub 2022 Jan 29. Eur Radiol. 2022. PMID: 35092473
Cited by
-
Baseline radiologic features as predictors of efficacy in patients with pancreatic neuroendocrine tumors with liver metastases receiving surufatinib.Chin J Cancer Res. 2023 Oct 30;35(5):526-535. doi: 10.21147/j.issn.1000-9604.2023.05.09. Chin J Cancer Res. 2023. PMID: 37969958 Free PMC article.
References
-
- Pavel M, Baudin E, Couvelard A, Krenning E, Öberg K, Steinmüller T, et al. . ENETS consensus guidelines for the management of patients with liver and other distant metastases from neuroendocrine neoplasms of foregut, midgut, hindgut, and unknown primary. Neuroendocrinology 2012; 95: 157–76. doi: 10.1159/000335597 - DOI - PubMed
-
- Steinmüller T, Kianmanesh R, Falconi M, Scarpa A, Taal B, Kwekkeboom DJ, et al. . Consensus guidelines for the management of patients with liver metastases from digestive (neuro)endocrine tumors: foregut, midgut, hindgut, and unknown primary. Neuroendocrinology 2008; 87: 47–62. doi: 10.1159/000111037 - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

