Incidence and risk factors for post-operative mortality, hospitalization, and readmission rates following pancreatic cancer resection
- PMID: 31949925
- PMCID: PMC6955019
- DOI: 10.21037/jgo.2019.09.01
Incidence and risk factors for post-operative mortality, hospitalization, and readmission rates following pancreatic cancer resection
Abstract
Background: The only potentially curative approach for pancreatic cancer is surgical resection, but this technically challenging procedure carries risks for postoperative morbidities and mortality. This study of a large, contemporary national database illustrates incidences of, and risk factors for, post-procedural mortality, prolonged hospital stay, and 30-day readmission.
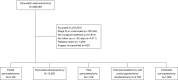
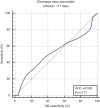
Methods: From the National Cancer Database (NCDB), stage I-III pancreatic adenocarcinomas were identified [2004-2015]. Surgical techniques included pancreaticoduodenectomy, partial pancreatectomy (selective removal of the pancreatic body/tail), total pancreatectomy (removal of the entire pancreas) with or without subtotal resection of the duodenum and/or stomach, and extended pancreatectomy. Predictors of 30/90-day post-operative mortality, 30-day readmission rates, and prolonged hospital stay (>17 days per receiver operating curve analysis) were identified via multivariable logistic regression.
Results: Overall, 24,798 patients were analyzed (median age of 66). The majority of cases were T3 (47%), N0 (65%), pancreatic head lesions (83%), and treated with pancreaticoduodenectomy (57%). Only 16% received neoadjuvant therapy. Overall unadjusted risk of 30- and 90-day mortality ranged from 1.3-2.5% and 4.1-7.1%, respectively, depending on extent of surgery. Independent predictors of 30-/90-day mortality included preoperative therapy, increasing age, higher comorbidity score, lower income, case volume, and more extensive surgery. Similar findings were demonstrated regarding prolonged hospital stay and 30-day readmission. Age ≥70 was most associated with 30-day mortality, whereas age ≥60 was most associated with 90-day mortality and prolonged hospital stay.
Conclusions: Quantitation of incidences and risk factors for postoperative outcomes following resection for pancreatic cancer is essential for judicious patient selection and shared decision-making between providers and patients.
Keywords: Pancreatic cancer; Whipple; pancreatectomy; pancreaticoduodenectomy.
2019 Journal of Gastrointestinal Oncology. All rights reserved.
Conflict of interest statement
Conflicts of Interest: The authors have no conflicts of interest to declare.
Figures


References
LinkOut - more resources
Full Text Sources
