Bioresorbable silk grafts for small diameter vascular tissue engineering applications: In vitro and in vivo functional analysis
- PMID: 31958596
- PMCID: PMC7050402
- DOI: 10.1016/j.actbio.2020.01.020
Bioresorbable silk grafts for small diameter vascular tissue engineering applications: In vitro and in vivo functional analysis
Abstract
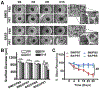
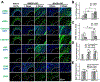
The success of tissue-engineered vascular graft (TEVG) predominantly relies on the selection of a suitable biomaterial and graft design. Natural biopolymer silk has shown great promise for various tissue-engineering applications. This study is the first to investigate Indian endemic non-mulberry silk (Antheraea assama-AA) - which inherits naturally superior mechanical and biological traits (e.g., RGD motifs) compared to Bombyx mori-BM silk, for TEVG applications. We designed bi-layered biomimetic small diameter AA-BM silk TEVGs adopting a new fabrication methodology. The inner layer showed ideally sized (~40 µm) pores with interconnectivity to allow cellular infiltration, and an outer dense electrospun layer that confers mechanical resilience. Biodegradation of silk TEVGs into amino acids as resorbable byproducts corroborates their in vivo remodeling ability. Following our previous reports, we surgically implanted human adipose tissue-derived stromal vascular fraction (SVF) seeded silk TEVGs in Lewis rats as abdominal aortic interposition grafts for 8 weeks. Adequate suture retention strength (0.45 ± 0.1 N) without any blood seepage post-implantation substantiate the grafts' viability. AA silk-based TEVGs showed superior animal survival and graft patency compared to BM silk TEVGs. Histological analysis revealed neo-tissue formation, host cell infiltration and graft remodeling in terms of extracellular matrix turnover. Altogether, this study demonstrates promising aspects of AA silk TEVGs for vascular tissue engineering applications. STATEMENT OF SIGNIFICANCE: Clinical 'off the shelf' implementation of tissue-engineered vascular grafts (TEVGs) remains a challenge. Achieving optimal blood vessel regeneration requires the use of bioresorbable materials having suitable degradation rates while producing minimal or no toxic byproducts. Host cell recruitment and preventing acute thrombosis are other pre-requisites for successful graft remodeling. In this study, for the first time we explored the use of naturally derived Indian endemic non-mulberry Antheraea assama silk in combination with Bombyx mori silk for TEVG applications by adopting a new biomimetic approach. Our bi-layered silk TEVGs were optimally porous, mechanically resilient and biodegradable. In vivo implantation in rat aorta showed long-term patency and graft remodeling by host cell infiltration and extracellular matrix deposition corroborating their clinical feasibility.
Keywords: Biodegradation; Non-mulberry silk; Tissue engineering; Tissue remodeling; Vascular grafts.
Copyright © 2020 Acta Materialia Inc. All rights reserved.
Conflict of interest statement
Declaration of Competing Interest The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Figures


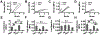
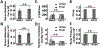



References
-
- Veith FJ, Moss CM, Sprayregen S, Montefusco C, Preoperative saphenous venography in arterial reconstructive surgery of the lower extremity, Surgery 85(3) (1979) 253–256. - PubMed
-
- Weinberg CB, Bell E, A blood vessel model constructed from collagen and cultured vascular cells, Science 231(4736) (1986) 397–400. - PubMed
-
- Shin’oka T, Imai Y, Ikada Y, Transplantation of a tissue-engineered pulmonary artery, New England Journal of Medicine 344(7) (2001) 532–533. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials

