Rate and risk factors for rehospitalisation in sepsis survivors: systematic review and meta-analysis
- PMID: 31974919
- PMCID: PMC7222906
- DOI: 10.1007/s00134-019-05908-3
Rate and risk factors for rehospitalisation in sepsis survivors: systematic review and meta-analysis
Abstract
Purpose: Sepsis survivors have a higher risk of rehospitalisation and of long-term mortality. We assessed the rate, diagnosis, and independent predictors for rehospitalisation in adult sepsis survivors.
Methods: We searched for non-randomized studies and randomized clinical trials in MEDLINE, Cochrane Library, Web of Science, and EMBASE (OVID interface, 1992-October 2019). The search strategy used controlled vocabulary terms and text words for sepsis and hospital readmission, limited to humans, and English language. Two authors independently selected studies and extracted data using predefined criteria and data extraction forms.
Results: The literature search identified 12,544 records. Among 56 studies (36 full and 20 conference abstracts) that met our inclusion criteria, all were non-randomised studies. Studies most often report 30-day rehospitalisation rate (mean 21.4%, 95% confidence interval [CI] 17.6-25.4%; N = 36 studies reporting 6,729,617 patients). The mean (95%CI) rehospitalisation rates increased from 9.3% (8.3-10.3%) by 7 days to 39.0% (22.0-59.4%) by 365 days. Infection was the most common rehospitalisation diagnosis. Risk factors that increased the rehospitalisation risk in sepsis survivors were generic characteristics such as older age, male, comorbidities, non-elective admissions, hospitalisation prior to index sepsis admission, and sepsis characteristics such as infection and illness severity, with hospital characteristics showing inconsistent associations. The overall certainty of evidence was moderate for rehospitalisation rates and low for risk factors.
Conclusions: Rehospitalisation events are common in sepsis survivors, with one in five rehospitalisation events occurring within 30 days of hospital discharge following an index sepsis admission. The generic and sepsis-specific characteristics at index sepsis admission are commonly reported risk factors for rehospitalisation.
Registration: PROSPERO CRD 42016039257, registered on 14-06-2016.
Keywords: Competing risk; Rehospitalisation; Risk factors; Sepsis.
Conflict of interest statement
The authors declare no conflict of interest directly applicable to this research.
Figures
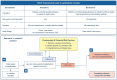


References
-
- Singer M, Deutschman CS, Seymour CW, Shankar-Hari M, Annane D, Bauer M, Bellomo R, Bernard GR, Chiche JD, Coopersmith CM, Hotchkiss RS, Levy MM, Marshall JC, Martin GS, Opal SM, Rubenfeld GD, van der Poll T, Vincent JL, Angus DC. The third International consensus definitions for sepsis and septic shock (sepsis-3) JAMA. 2016;315:801–810. - PMC - PubMed
-
- Reinhart K, Daniels R, Kissoon N, Machado FR, Schachter RD, Finfer S. Recognizing sepsis as a global health priority—a WHO resolution. N Engl J Med. 2017;377:414–417. - PubMed
-
- Shankar-Hari M, Harrison DA, Rubenfeld GD, Rowan K. Epidemiology of sepsis and septic shock in critical care units: comparison between sepsis-2 and sepsis-3 populations using a national critical care database. Br J Anaesth. 2017;119:626–636. - PubMed
-
- Kaukonen KM, Bailey M, Suzuki S, Pilcher D, Bellomo R. Mortality related to severe sepsis and septic shock among critically ill patients in Australia and New Zealand, 2000–2012. JAMA. 2014;311:1308–1316. - PubMed
-
- Fleischmann C, Scherag A, Adhikari NK, Hartog CS, Tsaganos T, Schlattmann P, Angus DC, Reinhart K, International Forum of Acute Care T Assessment of global incidence and mortality of hospital-treated sepsis. Current estimates and limitations. Am J Respir Crit Care Med. 2016;193:259–272. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

