Clinical magnetic resonance imaging of arthroplasty at 1.5 T
- PMID: 31975444
- PMCID: PMC7293946
- DOI: 10.1002/jor.24606
Clinical magnetic resonance imaging of arthroplasty at 1.5 T
Abstract
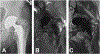
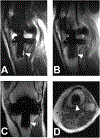
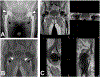
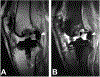
Magnetic resonance imaging (MRI) has historically been avoided for the routine clinical evaluation of metal implants at many clinical centers due to the presence of artifact that creates in-plane and through-plane distortions and signal intensity voids in generated images. However, when the image acquisition parameters are appropriately modified and advanced multi-spectral pulse sequences are used, high-quality diagnostic images can be generated and may be used for diagnosing patients with suspected periprosthetic pathology. MRI provides superior soft-tissue contrast and excellent sensitivity for mobile water and is, therefore, a valuable tool in the evaluation of these patients, given the increasing prevalence of arthroplasty within the general population. Knowledge of expected normal postoperative appearance in patients with total hip arthroplasty, total knee arthroplasty, and total shoulder arthroplasty facilitates the detection of abnormal findings in this population, as does familiarity with common pathologic conditions encountered in the periprosthetic region. This review article will provide background information regarding the presence of image artifacts, methods to reduce the artifacts, and application of MRI at 1.5 T for evaluating common complications in subjects with total knee arthroplasty, total hip arthroplasty, and total shoulder arthroplasty.
Keywords: adverse soft tissue reaction; arthroplasty; arthroplasty-hip; arthroplasty-knee; diagnostic imaging; implant fixation; implant wear.
© 2020 Orthopaedic Research Society. Published by Wiley Periodicals, Inc.
Figures
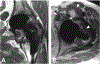

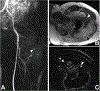


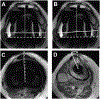

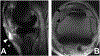
References
-
- Kurtz S, Ong K, Lau E, et al. 2007. Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. JBJS Am 89(4):780–785. - PubMed
-
- Barrack RL, Sawhney J, Hsu J, Cofield RH. 1999. Cost analysis of revision total hip arthroplasty. A 5-year followup study. CORR 369:175–178. - PubMed
-
- Saleh KJ, Thongtrangan I, Schwarz EM. 2004. Osteolysis: medical and surgical approaches. CORR (427):138–147. - PubMed
-
- Purdue PE, Koulouvaris P, Potter HG, et al. 2007. The cellular and molecular biology of periprosthetic osteolysis. CORR 454:251–261. - PubMed
-
- Southwell DG, Bechtold JE, Lew WD, Schmidt AH. 1999. Improving the detection of acetabular osteolysis using oblique radiographs. JBJS Br 81(2):289–295. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical

