Distinctive and common features of moderate aplastic anaemia
- PMID: 32004386
- PMCID: PMC8340733
- DOI: 10.1111/bjh.16460
Distinctive and common features of moderate aplastic anaemia
Abstract
The therapy algorithm for severe aplastic anaemia (sAA) is established but moderate AA (mAA), which likely reflects a more diverse pathogenic mechanism, often represents a treatment/management conundrum. A cohort of AA patients (n = 325) was queried for those with non-severe disease using stringent criteria including bone marrow hypocellularity and chronic persistence of moderately depressed blood counts. As a result, we have identified and analyzed pathological and clinical features in 85 mAA patients. Progression to sAA and direct clonal evolution (paroxysmal nocturnal haemoglobinuria/acute myeloid leukaemia; PNH/AML) occurred in 16%, 11% and 1% of mAA cases respectively. Of the mAA patients who received immunosuppressive therapy, 67% responded irrespective of time of initiation of therapy while conservatively managed patients showed no spontaneous remissions. Genomic analysis of mAA identified evidence of clonal haematopoiesis with both persisting and remitting patterns at low allelic frequencies; with more pronounced mutational burden in sAA. Most of the mAA patients have autoimmune pathogenesis similar to those with sAA, but mAA contains a mix of patients with diverse aetiologies. Although progression rates differed between mAA and sAA (P = 0·003), cumulative incidences of mortalities were only marginally different (P = 0·095). Our results provide guidance for diagnosis/management of mAA, a condition for which no current standard of care is established.
Keywords: acute myeloid leukaemia; clinical outcomes; moderate aplastic anaemia; molecular mutation; myelodysplastic syndrome.
© 2020 The Authors. British Journal of Haematology published by British Society for Haematology and John Wiley & Sons Ltd.
Conflict of interest statement
The authors declare to have no potential conflicts of interest regarding the present work.
Figures
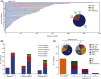

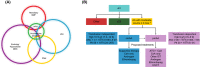
References
-
- Afable, M.G. 2nd , Tiu, R.V. & Maciejewski, J.P. (2011a) Clonal evolution in aplastic anemia. Hematology/the Education Program of the American Society of Hematology, 2011, 90–95. - PubMed
-
- Afable, M.G. 2nd , Wlodarski, M. , Makishima, H. , Shaik, M. , Sekeres, M.A. , Tiu, R.V. , Kalaycio, M. , O'Keefe, C.L. & Maciejewski, J.P. (2011b) SNP array‐based karyotyping: differences and similarities between aplastic anemia and hypocellular myelodysplastic syndromes. Blood, 117, 6876–6884. - PMC - PubMed
-
- Babushok, D.V. , Perdigones, N. , Perin, J.C. , Olson, T.S. , Ye, W. , Roth, J.J. , Lind, C. , Cattier, C. , Li, Y. , Hartung, H. , Paessler, M.E. , Frank, D.M. , Xie, H.M. , Cross, S. , Cockroft, J.D. , Podsakoff, G.M. , Monos, D. , Biegel, J.A. , Mason, P.J. & Bessler, M. (2015) Emergence of clonal hematopoiesis in the majority of patients with acquired aplastic anemia. Cancer Genetics, 208, 115–128. - PMC - PubMed
-
- Bacigalupo, A. , Hows, J. , Gluckman, E. , Nissen, C. , Marsh, J. , Van Lint, M.T. , Congiu, M. , De Planque, M.M. , Ernst, P. , McCann, S. , Ragavashar, A. , Frickhofen, N. , Wursch, A. , Marmont, A.M. & Gordon‐Smith, E.C. (1988) Bone marrow transplantation (BMT) versus immunosuppression for the treatment of severe aplastic anaemia (SAA): a report of the EBMT SAA working party. British Journal of Haematology, 70, 177–182. - PubMed
-
- Barrett, J. , Saunthararajah, Y. & Molldrem, J. (2000) Myelodysplastic syndrome and aplastic anemia: distinct entities or diseases linked by a common pathophysiology? Seminars in Hematology, 37, 15–29. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials

