Minimizing surgical blood loss at cesarean hysterectomy for placenta previa with evidence of placenta increta or placenta percreta: the state of play in 2020
- PMID: 32007492
- PMCID: PMC8725207
- DOI: 10.1016/j.ajog.2020.01.044
Minimizing surgical blood loss at cesarean hysterectomy for placenta previa with evidence of placenta increta or placenta percreta: the state of play in 2020
Abstract
The evolution of multidisciplinary team-based care for women with placenta accreta spectrum disorder has delivered stepwise improvements in clinical outcomes. Central to this overall goal is the ability to limit blood loss at surgery. Placement of inflatable balloons within the pelvic arteries, most commonly in the anterior divisions of the internal iliac arteries, became popular in many centers, at the expense of prolonging surgical care and with attendant risks of vascular injury. In tandem, the need to expose pelvic sidewall anatomy to safely identify the course of the ureters re-popularized the alternative strategy of ligating the same anterior divisions of the internal iliac arteries. With incremental gains in surgical expertise, described in 5 steps in this review, our teams have witnessed a steady decline in surgical blood loss. Nevertheless, a subset of women has the most severe form of placenta accreta spectrum, namely placenta previa-percreta. Such women are at risk of major hemorrhage during surgery from vessels arising outside the territories of the internal iliac arteries. These additional blood supplies, mostly from the external iliac arteries, pose significant risks of major blood loss even in experienced hands. To address this risk, some centers, principally in China, have adopted an approach of routinely placing an infrarenal aortic balloon, with both impressively low rates of blood loss and an ability to conserve the uterus by resecting the placenta with the affected portion of the uterine wall. We review these literature developments in the context of safely performing elective cesarean hysterectomy for placenta previa-percreta, the most severe placenta accreta spectrum disorder.
Keywords: cesarean hysterectomy; hemorrhage; infrarenal aortic balloon; internal iliac artery ligation; interventional radiology; magnetic resonance imaging; placenta accreta spectrum disorder.
Copyright © 2020 Elsevier Inc. All rights reserved.
Conflict of interest statement
The authors report no conflict of interest.
Figures
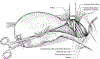
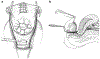
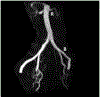
References
-
- Melcer Y, Jauniaux E, Maymon S, et al. Impact of targeted scanning protocols on peri-natal outcomes in pregnancies at risk of placenta accreta spectrum or vasa previa. Am J Obstet Gynecol 2018;218:443.e1–8. - PubMed
-
- Shamshirsaz AA, Fox KA, Erfani H, et al. Multidisciplinary team learning in the management of the morbidly adherent placenta: outcome improvements over time. Am J Obstet Gynecol 2017;216:612.e1–5. - PubMed
-
- Panaiotova J, Tokunaka M, Krajewska K, Zosmer N, Nicolaides KH. Screening for morbidly adherent placenta in early pregnancy. Ultrasound Obstet Gynecol 2019;53: 101–6. - PubMed
-
- Jauniaux E, Alfirevic Z, Bhide AG, et al. Placenta Praevia and placenta accreta: diagnosis and management: Green-top Guideline No. 27a. BJOG 2019;126:e1–48. - PubMed
-
- Hobson SR, Kingdom JC, Murji A, et al. No. 383—Screening, diagnosis, and management of placenta accreta spectrum disorders. J Obstet Gynaecol Can 2019;41:1035–49. - PubMed

