Association of Home Noninvasive Positive Pressure Ventilation With Clinical Outcomes in Chronic Obstructive Pulmonary Disease: A Systematic Review and Meta-analysis
- PMID: 32016309
- PMCID: PMC7042860
- DOI: 10.1001/jama.2019.22343
Association of Home Noninvasive Positive Pressure Ventilation With Clinical Outcomes in Chronic Obstructive Pulmonary Disease: A Systematic Review and Meta-analysis
Abstract
Importance: The association of home noninvasive positive pressure ventilation (NIPPV) with outcomes in chronic obstructive pulmonary disease (COPD) and hypercapnia is uncertain.
Objective: To evaluate the association of home NIPPV via bilevel positive airway pressure (BPAP) devices and noninvasive home mechanical ventilator (HMV) devices with clinical outcomes and adverse events in patients with COPD and hypercapnia.
Data sources: Search of MEDLINE, EMBASE, SCOPUS, Cochrane Central Registrar of Controlled Trials, Cochrane Database of Systematic Reviews, National Guideline Clearinghouse, and Scopus for English-language articles published from January 1, 1995, to November 6, 2019.
Study selection: Randomized clinical trials (RCTs) and comparative observational studies that enrolled adults with COPD with hypercapnia who used home NIPPV for more than 1 month were included.
Data extraction and synthesis: Data extraction was completed by independent pairs of reviewers. Risk of bias was evaluated using the Cochrane Collaboration risk of bias tool for RCTs and select items from the Newcastle-Ottawa Scale for nonrandomized studies.
Main outcomes and measures: Primary outcomes were mortality, all-cause hospital admissions, need for intubation, and quality of life at the longest follow-up.
Results: A total of 21 RCTs and 12 observational studies evaluating 51 085 patients (mean [SD] age, 65.7 [2.1] years; 43% women) were included, among whom there were 434 deaths and 27 patients who underwent intubation. BPAP compared with no device was significantly associated with lower risk of mortality (22.31% vs 28.57%; risk difference [RD], -5.53% [95% CI, -10.29% to -0.76%]; odds ratio [OR], 0.66 [95% CI, 0.51-0.87]; P = .003; 13 studies; 1423 patients; strength of evidence [SOE], moderate), fewer patients with all-cause hospital admissions (39.74% vs 75.00%; RD, -35.26% [95% CI, -49.39% to -21.12%]; OR, 0.22 [95% CI, 0.11-0.43]; P < .001; 1 study; 166 patients; SOE, low), and lower need for intubation (5.34% vs 14.71%; RD, -8.02% [95% CI, -14.77% to -1.28%]; OR, 0.34 [95% CI, 0.14-0.83]; P = .02; 3 studies; 267 patients; SOE, moderate). There was no significant difference in the total number of all-cause hospital admissions (rate ratio, 0.91 [95% CI, 0.71-1.17]; P = .47; 5 studies; 326 patients; SOE, low) or quality of life (standardized mean difference, 0.16 [95% CI, -0.06 to 0.39]; P = .15; 9 studies; 833 patients; SOE, insufficient). Noninvasive HMV use compared with no device was significantly associated with fewer all-cause hospital admissions (rate ratio, 0.50 [95% CI, 0.35-0.71]; P < .001; 1 study; 93 patients; SOE, low), but not mortality (21.84% vs 34.09%; RD, -11.99% [95% CI, -24.77% to 0.79%]; OR, 0.56 [95% CI, 0.29-1.08]; P = .49; 2 studies; 175 patients; SOE, insufficient). There was no statistically significant difference in the total number of adverse events in patients using NIPPV compared with no device (0.18 vs 0.17 per patient; P = .84; 6 studies; 414 patients).
Conclusions and relevance: In this meta-analysis of patients with COPD and hypercapnia, home BPAP, compared with no device, was associated with lower risk of mortality, all-cause hospital admission, and intubation, but no significant difference in quality of life. Noninvasive HMV, compared with no device, was significantly associated with lower risk of hospital admission, but there was no significant difference in mortality risk. However, the evidence was low to moderate in quality, the evidence on quality of life was insufficient, and the analyses for some outcomes were based on small numbers of studies.
Conflict of interest statement
Figures


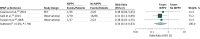

Comment in
-
Home Noninvasive Ventilation for Patients With Chronic Obstructive Pulmonary Disease and Chronic Respiratory Failure.JAMA. 2020 Feb 4;323(5):421-422. doi: 10.1001/jama.2019.22484. JAMA. 2020. PMID: 32016294 No abstract available.
-
Home noninvasive positive-pressure ventilation reduces mortality and intubations in COPD with hypercapnia.Ann Intern Med. 2020 Jun 16;172(12):JC64. doi: 10.7326/ACPJ202006160-064. Ann Intern Med. 2020. PMID: 32539518
-
Home Noninvasive Positive Pressure Ventilation for Chronic Obstructive Pulmonary Disease.JAMA. 2020 Jun 16;323(23):2432. doi: 10.1001/jama.2020.6090. JAMA. 2020. PMID: 32543679 No abstract available.
References
-
- Global Strategy for the Diagnosis, Management, and Prevention of Chronic Obstructive Pulmonary Disease. Fontina WI: Global Initiative for Chronic Obstructive Lung Disease; 2019. https://goldcopd.org/wp-content/uploads/2018/11/GOLD-2019-v1.7-FINAL-14N.... Accessed April 19, 2019.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

