Mild experimental increase in testis and epididymis temperature in men: effects on sperm morphology according to spermatogenesis stages
- PMID: 32038961
- PMCID: PMC6987600
- DOI: 10.21037/tau.2019.11.18
Mild experimental increase in testis and epididymis temperature in men: effects on sperm morphology according to spermatogenesis stages
Abstract
Background: A mild increase in testicular and epididymal temperatures in men, bulls and rams (pendulous scrotum) inhibits spermatogenesis and increases the percentage of sperm with an abnormal morphology. However, the stages of spermatogenesis that are most sensitive to a mild increase in testicular temperature in men are unknown. The aim of the present study was to explore the effects of a mild induced increase in testicular and epididymal temperature (i.e., testicular temperature maintained below the core body temperature) on sperm morphology in humans depending on the physiological time of spermatogenesis and epididymal transit.
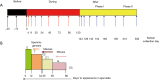
Methods: Five healthy volunteers were enrolled in an experimental study in which testicular and epididymal temperatures were increased by maintaining the testes in a supra-scrotal position with a specially designed underwear worn 15±1 h a day for 120 consecutive days. Semen collection was scheduled on specific days depending on spermatogenic stages and epididymal transit.
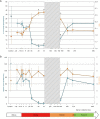
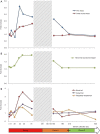
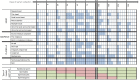
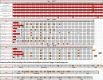
Results: Sperm morphology and the multiple anomalies index (MAI) were analysed before, during and after heating. This mild induced increase in testicular and epididymal temperatures resulted in a significant rise in the percentage of morphologically abnormal spermatozoa on day 34 of heating, which remained elevated throughout the heating period and persisted until 45 days after cessation of heating. The MAI was significantly increased on day 20 throughout the heating period and persisted 45 days after cessation of heating. An increase in the percentage of anomalies in the sperm head, acrosome or tail occurred on days 34 and/or 45 of heating. Abnormal sperm morphology and MAI reverted to control values 73 days after cessation of heating.
Conclusions: A mild sustained increase in testicular and epididymal temperature in man leads morphological abnormalities in spermatozoa mainly due to an impairment of spermiogenesis and meiosis.
Keywords: Men; meiosis; sperm morphology; spermiogenesis; testis temperature.
2019 Translational Andrology and Urology. All rights reserved.
Conflict of interest statement
Conflicts of Interest: The authors have no conflicts of interest to declare.
Figures
Similar articles
-
Experimental mild increase in testicular temperature has drastic, but reversible, effect on sperm aneuploidy in men: A pilot study.Reprod Biol. 2019 Jun;19(2):189-194. doi: 10.1016/j.repbio.2019.06.001. Epub 2019 Jun 14. Reprod Biol. 2019. PMID: 31208935 Clinical Trial.
-
Review: Testicular vascular cone development and its association with scrotal thermoregulation, semen quality and sperm production in bulls.Animal. 2018 Jun;12(s1):s133-s141. doi: 10.1017/S1751731118001167. Animal. 2018. PMID: 29882506 Review.
-
Twenty-four-hour monitoring of scrotal temperature in obese men and men with a varicocele as a mirror of spermatogenic function.Hum Reprod. 2015 May;30(5):1006-13. doi: 10.1093/humrep/dev057. Epub 2015 Mar 15. Hum Reprod. 2015. PMID: 25779699
-
The potential of mild testicular heating as a safe, effective and reversible contraceptive method for men.Int J Androl. 1994 Aug;17(4):186-91. doi: 10.1111/j.1365-2605.1994.tb01241.x. Int J Androl. 1994. PMID: 7995654
-
Possible physiological bases for contraceptive techniques in the male.Hum Reprod. 1994 Jun;9(6):1081-7. doi: 10.1093/oxfordjournals.humrep.a138637. Hum Reprod. 1994. PMID: 7962380 Review.
Cited by
-
Retinoic acid loaded with chitosan nanoparticles improves spermatogenesis in scrotal hyperthermia in mice.Clin Exp Reprod Med. 2023 Dec;50(4):230-243. doi: 10.5653/cerm.2023.06149. Epub 2023 Sep 8. Clin Exp Reprod Med. 2023. PMID: 37995751 Free PMC article.
-
Use of Infrared Thermography during Ejaculation Process and Its Link with Semen Quality and Freezability in Dogs.Animals (Basel). 2021 Oct 20;11(11):3023. doi: 10.3390/ani11113023. Animals (Basel). 2021. PMID: 34827755 Free PMC article.
-
Reconstruction of the Necrotic Scrotum with Hydrosurgery System and Pedicle DIEP Flap: A Case Report of Fournier Gangrene.Plast Reconstr Surg Glob Open. 2020 Sep 23;8(9):e3135. doi: 10.1097/GOX.0000000000003135. eCollection 2020 Sep. Plast Reconstr Surg Glob Open. 2020. PMID: 33133974 Free PMC article.
-
DNA damage in human sperm: The sperm chromosome assay.Reprod Med Biol. 2022 Apr 20;21(1):e12461. doi: 10.1002/rmb2.12461. eCollection 2022 Jan-Dec. Reprod Med Biol. 2022. PMID: 35475148 Free PMC article.
-
Effect of Temperature on the Development of Stages of Spermatogenesis and the Functionality of Sertoli Cells In Vitro.Int J Mol Sci. 2024 Feb 10;25(4):2160. doi: 10.3390/ijms25042160. Int J Mol Sci. 2024. PMID: 38396838 Free PMC article.
References
-
- Liu YX. Temperature control of spermatogenesis and prospect of male contraception. Front Biosci (Schol Ed) 2010;2:730-55. - PubMed
LinkOut - more resources
Full Text Sources
