Clinical study on surgical treatment of granulomatous lobular mastitis
- PMID: 32042679
- PMCID: PMC6989911
- DOI: 10.21037/gs.2019.11.12
Clinical study on surgical treatment of granulomatous lobular mastitis
Abstract
Background: The etiology and pathogenesis of granulomatous lobular mastitis (GLM) remain unknown, with no unified evaluation criteria or standard treatments. This study aimed to assess the etiology and features of GLM, as well as the effects of surgery (lesion excision + stage I breast reconstruction; LE + BR) for GLM.
Methods: This study evaluated 178 female GLM patients retrospectively in 2006-2015. The surgery and non-surgery groups included 164 and 14 patients, respectively. All patients received conservative therapy (traditional Chinese medicine combined with regional wet compress and pus drainage). In addition, the surgery group (n=164) underwent LE + BR. Clinical data, including disease course, causes, lesion size, marital status, and treatment approaches, were assessed.
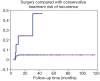
Results: Follow-up was 13-117 months. Seventy-five of the 178 patients had no overt causes (42.1%); meanwhile, 63 (35.4%) and 16 (9.0%) had congenital nipple retraction and a history of psychotropic drugs for >1 year, respectively. The surgery group showed lesions significantly shrunk (≤1 quadrant) with acute inflammation fully controlled; 8 showed recurrence, indicating a cure rate of 95.1% (156/164). In the non-surgery group, 4 cases showed relapse after 6-14 months (cure rate =71.4%; 10/14). Therefore, surgical treatment was significantly more efficient than non-surgical treatment (P=0.001). Kaplan-Meier survival curves for the two treatment types showed a significant difference in recurrence (log rank =11.84, P<0.001).
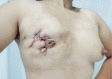
Conclusions: In GLM patients, LE + BR is safe and effective with respect to cosmetic results, recovery time, and recurrence. Successful surgery should be performed for patients whose lesions ≤1 quadrant, aim to achieve optimal GLM treatment.
Keywords: Conservative therapy; granulomatous lobular mastitis (GLM); intraglandular flap; predisposing factors; surgery.
2019 Gland Surgery. All rights reserved.
Conflict of interest statement
Conflicts of Interest: The authors have no conflicts of interest to declare.
Figures
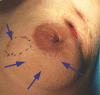
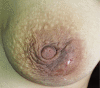
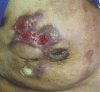
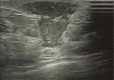








Comment in
-
Comment on: clinical study on surgical treatment of granulomatous lobular mastitis.Gland Surg. 2020 Aug;9(4):1065-1068. doi: 10.21037/gs-20-492. Gland Surg. 2020. PMID: 32953616 Free PMC article. No abstract available.
References
-
- Zhang C, Fan P, Yu H, et al. Surgical Treatment of Idiopathic Granulomatous Mastitis(8 cases report). Chinese Journal of General Surgery 2009;18:1216-9.
LinkOut - more resources
Full Text Sources
