Spatial clustering and determinants of home birth after at least one antenatal care visit in Ethiopia: Ethiopian demographic and health survey 2016 perspective
- PMID: 32046677
- PMCID: PMC7014695
- DOI: 10.1186/s12884-020-2793-6
Spatial clustering and determinants of home birth after at least one antenatal care visit in Ethiopia: Ethiopian demographic and health survey 2016 perspective
Abstract
Background: All pregnancies are at risk and have to be attended by skilled professionals. In Ethiopia however nearly half (45.7%) of the women were giving birth at home after antenatal care (ANC) visits in which skilled professionals were not available. Therefore, the aim of this study was to assess spatial clustering and the determinant factors of home delivery after antenatal care visits in Ethiopia.
Methods: A case control study was conducted on 2110 mothers who gave birth at home after ANC (cases), and 2510 mothers who gave birth at health institutions after attending ANC (controls), based on EDHS 2016 data. As per the recommendations of the DHS program, we weighed the data before analysis. ArcGIS 10.3 was used to show spatial pattern and SaTScan™ 9.4 to identify significant clusters. Stata 14 was used for data cleaning, weighing, and the analysis of the determinant factors. Bi variable and multi variable multilevel mixed effect logistic regression was fitted. Finally, the Log-likelihood ratio (LLR) and Relative risk with p-value of spatial scan statistics and AOR with 95% CI for significant determinant factors were reported.
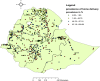
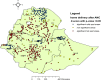
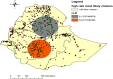
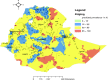
Results: Home delivery after ANC was spatially clustered in Ethiopia (Moran's Index = 0.91, p-value< 0.01). Attending, 1-3 ANC visits (AOR = 1.41, 95%CI: 1.17-1.71), no information about birth preparedness plan (AOR = 2.21, 95%CI: 1.83-2.69), pregnancies wanted later (AOR = 1.55, 95%CI: 1.20, 2.06), not having health insurance (AOR = 2.16, 95% CI: 1.29, 3.62), Muslim (AOR = 1.57, 95% CI: 1.13, 2.19) and protestant (AOR = 1.72, 95%CI: 1.16, 2.42) religions were positively associated with home delivery; While being rich (AOR = 0.42, 95%CI: 0.32-0.54), middle wealth index (AOR = O.66, 95%CI: 0.51, 0.86), primary education (AOR = 0.45, 95%CI: 0.36-0.55), secondary education (AOR = 0.11, 95%CI: 0.07-0.16), above secondary education (AOR = 0.06, 95%CI: 0.03-0.11) were negatively associated.
Conclusions: Home delivery after ANC follow ups was spatially clustered. Socio-demographic, health service and pregnancy related factors determined the prevalence of home delivery after antenatal care visits. Strengthening women's education, ANC visit, giving more information about birth preparedness plan, and improving family wealth are vital to reduce home delivery after antenatal care visits.
Keywords: Antenatal care; Ethiopia; Home delivery; Spatial distribution.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures

References
-
- World Health organization, Department of Maternal N, Child and adolescent health . Family, Women’s and Children’s Health Integrated Management Of Pregnancy And Childbirth. 2 2017.
-
- Global health obseervatory. Skilled birth attendant situations and trends. 2018. https://www.who.int/gho/maternal_health/skilled_care/skilled_birth_atten....
-
- WHO . SWIZERLAND Department of Maternal, Newborn, Child and Adolescent Health. 2018. WHO recommendations Intrapartum care for a positive childbirth experience. - PubMed
-
- WHO . WHO media center. 2016. maternal mortality fact sheet 2016.
-
- Kassebaum NJ, Barber RM, Bhutta ZA, Dandona L, Gething PW, Hay SI, et al. Global, regional, and national levels of maternal mortality, 1990–2015: a systematic analysis for the global burden of disease study 2015. Lancet. 2016;388(10053):1775–1812. doi: 10.1016/S0140-6736(16)31470-2. - DOI - PMC - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials

