Recurrence Patterns after Surgery in Patients with Different Endometriosis Subtypes: A Long-Term Hospital-Based Cohort Study
- PMID: 32054117
- PMCID: PMC7073694
- DOI: 10.3390/jcm9020496
Recurrence Patterns after Surgery in Patients with Different Endometriosis Subtypes: A Long-Term Hospital-Based Cohort Study
Abstract
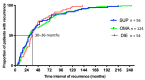
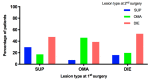
Recurrence of endometriosis after surgery constitutes a serious challenge. Whether there is an evolution of lesion subtypes with each recurrence and whether certain lesions subtypes tend to recur faster than others is not adequately addressed. Medical records of all patients who underwent surgery for endometriosis between 1997 and 2018 in the Department of Gynecology and Obstetrics, University of Bern, were reviewed. Inclusion criteria was surgically confirmed endometriosis recurrence, defined as a subsequent surgery for endometriosis after a previous complete surgical excision of endometriosis lesions. Three subtypes of endometriosis were defined: superficial peritoneal endometriosis (SUP), ovarian endometrioma (OMA), and deep infiltrating endometriosis (DIE). Time to recurrence and variation in endometriosis subtype between the first and recurrent surgeries were the primary outcome measures. Out of the 322 patients with recurrent surgery that were identified, for 234 of them, the endometriosis subtype at first surgery was confirmed and classified (SUP = 56, OMA = 124, DIE = 54). No statistically significant difference was found for time to recurrence between lesion subtypes. SUP compared to the other groups had a higher possibility of presenting with SUP at recurrence (Odds Ratio (OR): 3.65, 95% confidence interval (CI): 1.74-7.51) and OMA compared to the other groups had a higher possibility of presenting with OMA at recurrence (OR: 3.72, 95% CI: 2.04-6.74). Nevertheless, a large number of SUP patients subsequently presented with OMA (10/56: 17.9%) or DIE (27/56: 48.2%) lesions at recurrence. Similarly, a large number of OMA patients subsequently presented with DIE (49/124: 39.5%) lesions at recurrence. In conclusion, although SUP and OMA patients compared to the others are more likely to present with the same subtype at recurrence, increasing lesion subtype severity occurs in a substantial proportion of patients. Time to recurrence is independent from the lesion subtype at first surgery.
Keywords: deep-infiltrative endometriosis; endometrioma; peritoneal endometriosis; progression; recurrence.
Conflict of interest statement
Authors Nirgianakis, Ma, McKinnon and Mueller have no conflicts of interest or financial ties to disclose.
Figures
References
-
- Vercellini P., Fedele L., Aimi G., Pietropaolo G., Consonni D., Crosignani P.G. Association between endometriosis stage, lesion type, patient characteristics and severity of pelvic pain symptoms: A multivariate analysis of over 1000 patients. Hum. Reprod. 2007;22:266–271. doi: 10.1093/humrep/del339. - DOI - PubMed
LinkOut - more resources
Full Text Sources

