Neonatal Mortality After Interhospital Transfer of Pregnant Women for Imminent Very Preterm Birth in Illinois
- PMID: 32065614
- PMCID: PMC7042951
- DOI: 10.1001/jamapediatrics.2019.6055
Neonatal Mortality After Interhospital Transfer of Pregnant Women for Imminent Very Preterm Birth in Illinois
Abstract
Importance: Reducing neonatal mortality is a national health care priority. Understanding the association between neonatal mortality and antenatal transfer of pregnant women to a level III perinatal hospital for delivery of infants who are very preterm (VPT) may help identify opportunities for improvement.
Objective: To assess whether antenatal transfer to a level III hospital is associated with neonatal mortality in infants who are VPT.
Design, setting, and participants: This population-based cross-sectional study included infants who were born VPT to Illinois residents in Illinois perinatal-network hospitals between January 1, 2015, and December 31, 2016, and followed up for 28 days after birth. Data analysis was conducted from June 2017 to September 2018.
Exposures: Delivery of an infant who was VPT at a (1) level III hospital after maternal presentation at that hospital (reference group), (2) a level III hospital after antenatal (in utero) transfer from another hospital, or (3) a non-level III hospital.
Main outcomes and measures: Neonatal mortality.
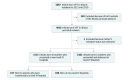
Results: The study included 4817 infants who were VPT (gestational age, 22-31 completed weeks) and were born to Illinois residents in 2015 and 2016. Of those, 3302 infants (68.5%) were born at a level III hospital after maternal presentation at that hospital, 677 (14.1%) were born at a level III hospital after antenatal transfer, and 838 (17.4%) were born at a non-level III hospital. Neonatal mortality for all infants who were VPT included in this study was 573 of 4817 infants (11.9%). The neonatal mortality was 10.7% for the reference group (362 of 3302 infants), 9.8% for the antenatal transfer group (66 of 677 infants), and 17.3% for the non-level III birth group (145 of 838 infants). When adjusted for significant social and medical characteristics, infants born VPT at a level III hospital after antenatal transfer from another facility had a similar risk of neonatal mortality as infants born at a level III hospital (odds ratio, 0.79 [95% CI, 0.56-1.13]) after maternal presentation at the same hospital. Infants born at a non-level III hospital had an increased risk of neonatal mortality compared with infants born at a level III hospital after maternal presentation to the same hospital (odds ratio, 1.52 [95% CI, 1.14-2.02]).
Conclusions and relevance: The risk of neonatal mortality was similar for infants who were VPT, whether women initially presented at a level III hospital or were transferred to a level III hospital before delivery. This suggests that the increased risk of mortality associated with delivery at a non-level III hospital may be mitigated by optimizing opportunities for early maternal transfer to a level III hospital.
Conflict of interest statement
Figures
Comment in
-
Delivering Neonates at High Risk in the Right Place: Back to the Future Again.JAMA Pediatr. 2020 Apr 1;174(4):329-330. doi: 10.1001/jamapediatrics.2019.6059. JAMA Pediatr. 2020. PMID: 32065605 No abstract available.
References
-
- Healthy People 2020 Maternal, infant, and child health. https://www.healthypeople.gov/2020/topics-objectives/topic/maternal-infa.... Accessed June 26, 2018.
-
- National Institute for Children’s Health Quality Collaborative Improvement and Innovation Network to Reduce Infant Mortality (Infant Mortality CoIIN). https://www.nichq.org/project/collaborative-improvement-and-innovation-n.... Accessed November 11, 2017.
-
- Illinois Department of Public Health Perinatal regionalization. http://www.dph.illinois.gov/topics-services/life-stages-populations/infa.... Accessed November 7, 2017.
-
- World Health Organization Neonatal mortality. https://www.who.int/gho/child_health/mortality/neonatal/en/. Accessed August 18, 2018.

