Hip resurfacing arthroplasty for osteonecrosis of the femoral head: Implant-specific outcomes and risk factors for failure
- PMID: 32071874
- PMCID: PMC7016032
- DOI: 10.1016/j.jot.2019.12.005
Hip resurfacing arthroplasty for osteonecrosis of the femoral head: Implant-specific outcomes and risk factors for failure
Abstract
Background: Hip resurfacing arthroplasty (HRA) may be a suitable option for treating osteonecrosis of the femoral head (ONFH). However, concerns regarding the extent of osteonecrosis, amount of defect under the prosthesis, and implant-related complications remain. This study aimed to report implant-specific outcomes and risk factors for failure of HRA in ONFH.
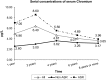
Methods: A total of 202 HRAs (166 patients) performed by a single surgeon were investigated. The stage, size, and location of ONFH were evaluated using preoperative radiographs and magnetic resonance images. Clinical, radiographic results, and serum metal concentrations of articular surface replacement (ASR) and non-ASR devices were compared. Logistic regression analysis was performed to identify the contributors of failures. The mean follow-up duration was 10.6 years.
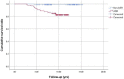
Results: Twenty-six hips (12.9%) were operated with Birmingham Hip Resurfacing (BHR), 99 (49.0%) with ASR, and 77 (38.1%) with Conserve Plus. The mean Harris Hip Score improved from 52.1 to 93.2 at the final follow-up (P < 0.001). Revision-free survivorships of non-ASR and ASR implants were 99.0% and 82.4%, respectively (P < 0.001). In multivariate analysis, the use of ASR prosthesis, greater combined necrotic angle, and smaller head size were associated with revision surgery. A large combined necrotic angle was the only independent risk factor for mechanical failure at the femoral side (P = 0.029).
Conclusion: HRA for ONFH using BHR and Conserve Plus implants demonstrated favourable clinical outcomes with high revision-free survival rates at 10 years. However, care should be taken for large necrotic lesions that can lead to femoral neck fracture or aseptic femoral loosening.
The translational potential of this article: This study suggests HRA performed for appropriately selected patients with ONFH can show excellent long-term clinical results. Therefore, HRA should remain as one of the treatment options for ONFH, and further development of HRA implants should be continued.
Keywords: Hip resurfacing arthroplasty; Implant-specific outcome; Mechanical failure; Osteonecrosis of the femoral head; Risk factors.
© 2019 The Author(s).
Conflict of interest statement
YSP is a paid consultant for Depuy Synthes.
Figures



References
-
- Haddad F.S., Konan S., Tahmassebi J. A prospective comparative study of cementless total hip arthroplasty and hip resurfacing in patients under the age of 55 years: a ten-year follow-up. Bone Joint Lett J. 2015;97-b:617–622. - PubMed
-
- Murray D.W., Grammatopoulos G., Pandit H., Gundle R., Gill H.S., McLardy-Smith P. The ten-year survival of the Birmingham hip resurfacing: an independent series. J Bone Joint Surg Br. 2012;94:1180–1186. - PubMed
-
- Baker R.P., Pollard T.C., Eastaugh-Waring S.J., Bannister G.C. A medium-term comparison of hybrid hip replacement and Birmingham hip resurfacing in active young patients. J Bone Joint Surg Br. 2011;93:158–163. - PubMed
-
- Cadossi M., Tedesco G., Sambri A., Mazzotti A., Giannini S. Hip resurfacing implants. Orthopedics. 2015;38:504–509. - PubMed
-
- Amstutz H.C., Le Duff M.J. Hip resurfacing: history, current status, and future. Hip Int. 2015;25:330–338. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

