Effect of dose and duration of reduction in dietary sodium on blood pressure levels: systematic review and meta-analysis of randomised trials
- PMID: 32094151
- PMCID: PMC7190039
- DOI: 10.1136/bmj.m315
Effect of dose and duration of reduction in dietary sodium on blood pressure levels: systematic review and meta-analysis of randomised trials
Abstract
Objective: To examine the dose-response relation between reduction in dietary sodium and blood pressure change and to explore the impact of intervention duration.
Design: Systematic review and meta-analysis following PRISMA guidelines.
Data sources: Ovid MEDLINE(R), EMBASE, and Cochrane Central Register of Controlled Trials (Wiley) and reference lists of relevant articles up to 21 January 2019.
Inclusion criteria: Randomised trials comparing different levels of sodium intake undertaken among adult populations with estimates of intake made using 24 hour urinary sodium excretion.
Data extraction and analysis: Two of three reviewers screened the records independently for eligibility. One reviewer extracted all data and the other two reviewed the data for accuracy. Reviewers performed random effects meta-analyses, subgroup analyses, and meta-regression.
Results: 133 studies with 12 197 participants were included. The mean reductions (reduced sodium v usual sodium) of 24 hour urinary sodium, systolic blood pressure (SBP), and diastolic blood pressure (DBP) were 130 mmol (95% confidence interval 115 to 145, P<0.001), 4.26 mm Hg (3.62 to 4.89, P<0.001), and 2.07 mm Hg (1.67 to 2.48, P<0.001), respectively. Each 50 mmol reduction in 24 hour sodium excretion was associated with a 1.10 mm Hg (0.66 to 1.54; P<0.001) reduction in SBP and a 0.33 mm Hg (0.04 to 0.63; P=0.03) reduction in DBP. Reductions in blood pressure were observed in diverse population subsets examined, including hypertensive and non-hypertensive individuals. For the same reduction in 24 hour urinary sodium there was greater SBP reduction in older people, non-white populations, and those with higher baseline SBP levels. In trials of less than 15 days' duration, each 50 mmol reduction in 24 hour urinary sodium excretion was associated with a 1.05 mm Hg (0.40 to 1.70; P=0.002) SBP fall, less than half the effect observed in studies of longer duration (2.13 mm Hg; 0.85 to 3.40; P=0.002). Otherwise, there was no association between trial duration and SBP reduction.
Conclusions: The magnitude of blood pressure lowering achieved with sodium reduction showed a dose-response relation and was greater for older populations, non-white populations, and those with higher blood pressure. Short term studies underestimate the effect of sodium reduction on blood pressure.
Systematic review registration: PROSPERO CRD42019140812.
Published by the BMJ Publishing Group Limited. For permission to use (where not already granted under a licence) please go to http://group.bmj.com/group/rights-licensing/permissions.
Conflict of interest statement
Competing interests: All authors have completed the ICMJE uniform disclosure form at www.icmje.org/coi_disclosure.pdf and declare: no support from any organisation for the submitted work. Outside this work, BN has received salt substitute for trials from Salt Manufacturing Company in China and Nutek; MW is supported by the National Health and Medical Research Foundation of Australia grants (1080206 and 1149987) and receives personal fees from Amgen, personal fees from Kirin; NRCC is an unpaid member of World Action on Salt and Health and an unpaid consultant on dietary sodium and hypertension control to numerous governmental and non-governmental organisations; AAL is funded by the Hypertension Canada New Investigator Award; FJH is a member of Consensus Action on Salt and Health (CASH) and World Action on Salt and Health (WASH). Both CASH and WASH are non-profit charitable organisations and FJH does not receive any financial support from CASH or WASH; GAM is the Chairman of Blood Pressure UK (BPUK), Chairman of Consensus Action on Salt and Health (CASH) and Chairman of World Action on Salt and Health (WASH). BPUK, CASH and WASH are non-profit charitable organisations and GAM does not receive any financial support from any of these organisations.
Figures
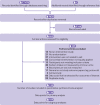




References
-
- GBD 2017 Causes of Death Collaborators Global, regional, and national age-sex-specific mortality for 282 causes of death in 195 countries and territories, 1980-2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 2018;392:1736-88. 10.1016/S0140-6736(18)32203-7 - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
