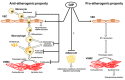
GIP as a Potential Therapeutic Target for Atherosclerotic Cardiovascular Disease-A Systematic Review
- PMID: 32098413
- PMCID: PMC7073149
- DOI: 10.3390/ijms21041509
GIP as a Potential Therapeutic Target for Atherosclerotic Cardiovascular Disease-A Systematic Review
Abstract
Glucose-dependent insulinotropic polypeptide (GIP) and glucagon-like peptide-1 (GLP-1) are gut hormones that are secreted from enteroendocrine L cells and K cells in response to digested nutrients, respectively. They are also referred to incretin for their ability to stimulate insulin secretion from pancreatic beta cells in a glucose-dependent manner. Furthermore, GLP-1 exerts anorexic effects via its actions in the central nervous system. Since native incretin is rapidly inactivated by dipeptidyl peptidase-4 (DPP-4), DPP-resistant GLP-1 receptor agonists (GLP-1RAs), and DPP-4 inhibitors are currently used for the treatment of type 2 diabetes as incretin-based therapy. These new-class agents have superiority to classical oral hypoglycemic agents such as sulfonylureas because of their low risks for hypoglycemia and body weight gain. In addition, a number of preclinical studies have shown the cardioprotective properties of incretin-based therapy, whose findings are further supported by several randomized clinical trials. Indeed, GLP-1RA has been significantly shown to reduce the risk of cardiovascular and renal events in patients with type 2 diabetes. However, the role of GIP in cardiovascular disease remains to be elucidated. Recently, pharmacological doses of GIP receptor agonists (GIPRAs) have been found to exert anti-obesity effects in animal models. These observations suggest that combination therapy of GLP-1R and GIPR may induce superior metabolic and anti-diabetic effects compared with each agonist individually. Clinical trials with GLP-1R/GIPR dual agonists are ongoing in diabetic patients. Therefore, in this review, we summarize the cardiovascular effects of GIP and GIPRAs in cell culture systems, animal models, and humans.
Keywords: GIP; animal model; atherosclerosis; cardiac remodeling; restenosis.
Conflict of interest statement
There is no conflict of interest to be disclosed.
Figures
References
-
- Wang C.C.L., Hess C.N., Hiatt W.R., Goldfine A.B. Clinical Update: Cardiovascular Disease in Diabetes Mellitus: Atherosclerotic Cardiovascular Disease and Heart Failure in Type 2 Diabetes Mellitus—Mechanisms, Management, and Clinical Considerations. Circulation. 2016;133:2459–2502. doi: 10.1161/CIRCULATIONAHA.116.022194. - DOI - PMC - PubMed
-
- Nathan D.M., Cleary P.A., Backlund J.Y., Genuth S.M., Lachin J.M., Orchard T.J., Raskin P., Zinman B., Diabetes Control and Complications Trial/Epidemiology of Diabetes Interventions and Complications (DCCT/EDIC) Study Research Group Intensive diabetes treatment and cardiovascular disease in patients with type 1 diabetes. N. Engl. J. Med. 2005;353:2643–2653. - PMC - PubMed
-
- Action to Control Cardiovascular Risk in Diabetes Study Group. Gerstein H.C., Miller M.E., Byington R.P., Goff D.C., Jr., Bigger J.T., Buse J.B., Cushman W.C., Genuth S., Ismail-Beigi F., et al. Effects of intensive glucose lowering in type 2 diabetes. N. Engl. J. Med. 2008;358:2545–2559. - PMC - PubMed
-
- ADVANCE Collaborative Group. Patel A., MacMahon S., Chalmers J., Neal B., Billot L., Woodward M., Marre M., Cooper M., Glasziou P., et al. Intensive blood glucose control and vascular outcomes in patients with type 2 diabetes. N. Engl. J. Med. 2008;358:2560–2572. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous