Using the BODE Index and Comorbidities to Predict Health Utilization Resources in Chronic Obstructive Pulmonary Disease
- PMID: 32110007
- PMCID: PMC7036670
- DOI: 10.2147/COPD.S234363
Using the BODE Index and Comorbidities to Predict Health Utilization Resources in Chronic Obstructive Pulmonary Disease
Abstract
Background and objective: Chronic Obstructive Pulmonary Disease (COPD) is a common chronic respiratory disease that in the long term may develop into respiratory failure or even cause death and may coexist with other diseases. Over time, it may incur huge medical expenses, resulting in a heavy socio-economy burden. The BODE (Body mass index, airflow Obstruction, Dyspnea, and Exercise capacity) index is a predictor of the number and severity of acute exacerbations of COPD. This study focused on the correlation between the BODE index, comorbidity, and healthcare resource utilization in COPD.
Patients and methods: This is a retrospective study of clinical outcomes of COPD patients with complete BODE index data in our hospital from January 2015 to December 2016. Based on the patients' medical records in our hospital's electronic database from January 1, 2015 to August 31, 2017, we analyzed the correlation between BODE index, Charlson comorbidity index (CCI), and medical resources.
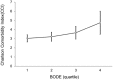
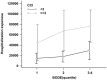
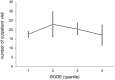
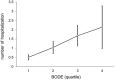
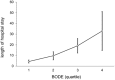
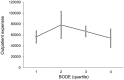
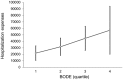
Results: Of the 396 patients with COPD who met the inclusion criteria, 382 (96.5%) were male, with an average age of 71.3 ± 8.4 years. Healthcare resource utilization was positively correlated with the BODE index during the 32 months of retrospective clinical outcomes. The study found a significant association between the BODE index and the CCI of COPD patients (p < 0.001). In-hospitalization expenses were positively correlated with CCI (p < 0.001). Under the same CCI, the higher the quartile, the higher the hospitalization expenses. BODE quartiles were positively correlated with number of hospitalizations (p < 0.001), hospitalization days (p < 0.001), hospitalization expenses (p = 0.005), and total medical expenses (p = 0.024).
Conclusion: This study demonstrates the value of examining the BODE index and comorbidities that can predict healthcare resource utilization in COPD.
Keywords: 6 min walk test; BODE index; Charlson comorbidity index; chronic obstructive pulmonary disease; medical burden.
© 2020 Li et al.
Conflict of interest statement
The authors report no conflicts of interest in this work.
Figures


Similar articles
-
The Relationship between Exertional Desaturation and Pulmonary Function, Exercise Capacity, or Medical Costs in Chronic Obstructive Pulmonary Disease Patients.Medicina (Kaunas). 2023 Feb 17;59(2):391. doi: 10.3390/medicina59020391. Medicina (Kaunas). 2023. PMID: 36837592 Free PMC article.
-
The DOSE index in chronic obstructive pulmonary disease: evaluating healthcare costs.BMC Pulm Med. 2024 Nov 8;24(1):560. doi: 10.1186/s12890-024-03368-0. BMC Pulm Med. 2024. PMID: 39516765 Free PMC article.
-
A multidimensional grading system (BODE index) as predictor of hospitalization for COPD.Chest. 2005 Dec;128(6):3810-6. doi: 10.1378/chest.128.6.3810. Chest. 2005. PMID: 16354849
-
Outcome measures in chronic obstructive pulmonary disease (COPD): strengths and limitations.Respir Res. 2010 Jun 17;11(1):79. doi: 10.1186/1465-9921-11-79. Respir Res. 2010. PMID: 20565728 Free PMC article. Review.
-
Predictors of mortality in COPD.Respir Med. 2010 Jun;104(6):773-9. doi: 10.1016/j.rmed.2009.12.017. Epub 2010 Apr 22. Respir Med. 2010. PMID: 20417082 Review.
Cited by
-
The Relationship between Exertional Desaturation and Pulmonary Function, Exercise Capacity, or Medical Costs in Chronic Obstructive Pulmonary Disease Patients.Medicina (Kaunas). 2023 Feb 17;59(2):391. doi: 10.3390/medicina59020391. Medicina (Kaunas). 2023. PMID: 36837592 Free PMC article.
-
Association Between Air Pollution and Lung Lobar Emphysema in COPD.Front Med (Lausanne). 2021 Sep 21;8:705792. doi: 10.3389/fmed.2021.705792. eCollection 2021. Front Med (Lausanne). 2021. PMID: 34621758 Free PMC article.
-
Chronic Obstructive Pulmonary Disease and Metabolic Syndrome: A Maltese Study on Biomarkers and Clinical Implications.Diabetes Metab Syndr Obes. 2025 Jul 21;18:2463-2476. doi: 10.2147/DMSO.S515061. eCollection 2025. Diabetes Metab Syndr Obes. 2025. PMID: 40726502 Free PMC article.
-
Survival following lung volume reduction procedures: results from the UK Lung Volume Reduction (UKLVR) registry.BMJ Open Respir Res. 2024 Feb 29;11(1):e002092. doi: 10.1136/bmjresp-2023-002092. BMJ Open Respir Res. 2024. PMID: 38423954 Free PMC article.
-
Correlation of BODE index with quality of life in stable Chronic Obstructive Pulmonary Disease (COPD) patients - A prospective study.J Family Med Prim Care. 2020 Nov 30;9(11):5606-5613. doi: 10.4103/jfmpc.jfmpc_735_20. eCollection 2020 Nov. J Family Med Prim Care. 2020. PMID: 33532403 Free PMC article.
References
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

