Individualized Prediction of Survival Benefit From Locoregional Surgical Treatment for Patients With Metastatic Breast Cancer
- PMID: 32133290
- PMCID: PMC7040087
- DOI: 10.3389/fonc.2020.00148
Individualized Prediction of Survival Benefit From Locoregional Surgical Treatment for Patients With Metastatic Breast Cancer
Erratum in
-
Corrigendum: Individualized Prediction of Survival Benefit From Locoregional Surgical Treatment for Patients With Metastatic Breast Cancer.Front Oncol. 2020 Apr 9;10:482. doi: 10.3389/fonc.2020.00482. eCollection 2020. Front Oncol. 2020. PMID: 32328463 Free PMC article.
Abstract
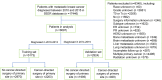
Objective: Recently, performing locoregional surgical treatment still remains debatable in patients with metastatic breast cancer (MBC). Current study aimed to develop prognostic nomograms for predicting the long-term survival in MBC patients with or without surgical intervention, thereby assisting clinicians in making individualized choice. Methods: The training set included 5173 patients who were diagnosed with MBC in 2010-2013 from the Surveillance, Epidemiology, and End Results Program, while the validation set comprised 2924 patients diagnosed in 2014-2015. Multivariant Cox hazard model was applied to determine the independent risk factors for overall survival (OS) and breast cancer specific survival (BCSS). Then, individualized pre- and postoperative nomograms for predicting 1- or 3-year survival probabilities were constructed accordingly. Internal and external validations were conducted to determine the accuracy of these nomograms by calculating concordance index (C-index) and plotting calibration curves. Results: The survival analysis indicated that surgical management conferred improved OS and BCSS in patients with metastatic breast cancer. Age, T stage, grade, distant metastatic site, ER, PR and HER2 status, radiation, and chemotherapy were independent risk factors for OS and BCSS both in surgery and non-surgery group. All these factors were subsequently incorporated into the nomogram which showed acceptable predictive capabilities with C-index range of 0.65-0.80 both in training set and external validation set. In addition, a preoperative nomogram incorporating variables capable of being determined before surgery was also built with C-index above 0.70 both in training and validation set. Conclusion: Surgical management in patients with metastatic breast cancer suggests a potential survival advantage. In addition, these well-validated pre- and postoperative nomograms may provide a useful tool to assist clinicians in treatment decision-making and in evaluating patients' long term prognosis.
Keywords: SEER program; clinic utility; metastatic breast cancer; nomogram; prognosis.
Copyright © 2020 Zheng, Zhong, Yu, Lei and Yang.
Figures



References
-
- Noone AM, Howlader N, Krapcho M, Miller D, Brest A, Yu M, et al. SEER Cancer Statistics Review, 1975-2015. Bethesda, MD: National Cancer Institute; Available online at: https://seer.cancer.gov/ (2018).
-
- Network. NCC (NCCN) Clinical Practice Guidelines in Oncology. Breast Cancer, Version 1. 2019. Available online at: https://www.nccn.org/about/permissions/reference.aspx (2019). (accessed Febraury 6, 2020).
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous

