Standard Versus Ultrasound-Guided Cannulation of the Femoral Artery in Patients Undergoing Invasive Procedures: A Meta-Analysis of Randomized Controlled Trials
- PMID: 32138283
- PMCID: PMC7141204
- DOI: 10.3390/jcm9030677
Standard Versus Ultrasound-Guided Cannulation of the Femoral Artery in Patients Undergoing Invasive Procedures: A Meta-Analysis of Randomized Controlled Trials
Abstract
Background: It is unclear whether or not ultrasound-guided cannulation (UGC) of the femoral artery is superior to the standard approach (SA) in reducing vascular complications and improving access success.
Objective: We sought to compare procedural and clinical outcomes of femoral UGC versus SA in patients undergoing percutaneous cardiovascular intervention (PCvI).
Methods: We searched EMBASE, MEDLINE, Scopus and web sources for randomized trials comparing UGC versus SA. We estimated risk ratio (RR) and standardized mean differences (SMDs) with 95% confidence intervals (CIs) for categorical and continuous variables, respectively. Primary efficacy endpoint was the success rate at the first attempt, while secondary efficacy endpoints were access time and number of attempts. Primary safety endpoints were the rates of vascular complications, while secondary endpoints were major bleeding, as well as access site hematoma, venepuncture, pseudoaneurysms and retroperitoneal hematoma. This meta-analysis has been registered on Centre for Open Science (OSF) (osf.io/fy82e).
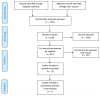
Results: Seven trials were included, randomizing 3180 patients to UGC (n = 1564) or SA (n = 1616). Efficacy between UGC and SA was the main metric assessed in most of the trials, in which one third of the enrolled patients underwent interventional procedures. The success rate of the first attempt was significantly higher with UGC compared to SA, (82.0% vs. 58.7%; RR: 1.36; 95% CI: 1.17 to 1.57; p < 0.0001; I2 = 88%). Time to access and number of attempts were significantly reduced with UGC compared to SA (SMD: -0.19; 95% CI: -0.28 to -0.10; p < 0.0001; I2 = 22%) and (SMD: -0.40; 95% CI: -0.58 to -0.21; p < 0.0001; I2 = 82%), respectively. Compared with SA, use of UGC was associated with a significant reduction in vascular complications (1.3% vs. 3.0%; RR: 0.48; CI 95%: 0.25 to 0.91; p = 0.02; I2 = 0%) and access-site hematoma (1.2% vs. 3.3%; RR: 0.41; CI 95%: 0.20 to 0.83; p = 0.01; I2 = 27%), but there were non-significant differences in major bleeding (0.7% vs. 1.4%; RR: 0.57; CI 95%: 0.24 to 1.32; p = 0.19; I2 = 0%). Rates of venepuncture were lower with UGC (3.6% vs. 12.1%; RR: 0.32; CI 95%: 0.20 to 0.52; p < 0.00001; I2 = 55%).
Conclusion: This study, which included all available data to date, demonstrated that, compared to a standard approach, ultrasound-guided cannulation of the femoral artery is associated with lower access-related complications and higher efficacy rates. These results could be of great clinical relevance especially in the femoral cannulation of high risk patients.
Keywords: bleeding; femoral artery; ultrasound; vascular complications.
Conflict of interest statement
The authors have no conflicts of interest to declare.
Figures



References
-
- Doyle B.J., Ting H.H., Bell M.R., Lennon R.J., Mathew V., Singh M., Holmes D.R., Rihal C.S. Major femoral bleeding complications after percutaneous coronary intervention: Incidence, predictors, and impact on long-term survival among 17,901 patients treated at the Mayo Clinic from 1994 to 2005. JACC Cardiovasc. Interv. 2008;1:202–209. doi: 10.1016/j.jcin.2007.12.006. - DOI - PubMed
-
- Neumann F.J., Sousa-Uva M., Ahlsson A., Alfonso F., Banning A.P., Benedetto U., Byrne R.A., Collet J.P., Falk V., Head S.J., et al. [2018 ESC/EACTS Guidelines on myocardial revascularization. The Task Force on myocardial revascularization of the European Society of Cardiology (ESC) and European Association for Cardio-Thoracic Surgery (EACTS)] G. Ital. Cardiol. 2019;20:1–61. - PubMed
-
- Jolly S.S., Yusuf S., Cairns J., Niemelä K., Xavier D., Widimsky P., Budaj A., Niemelä M., Valentin V., Lewis B.S., et al. Radial versus femoral access for coronary angiography and intervention in patients with acute coronary syndromes (RIVAL): A randomised, parallel group, multicentre trial. Lancet. 2011;377:1409–1420. doi: 10.1016/S0140-6736(11)60404-2. - DOI - PubMed
LinkOut - more resources
Full Text Sources

