Salivary Cortisol Determination on Smartphone-Based Differential Pulse Voltammetry System
- PMID: 32150916
- PMCID: PMC7085790
- DOI: 10.3390/s20051422
Salivary Cortisol Determination on Smartphone-Based Differential Pulse Voltammetry System
Abstract
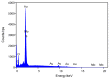
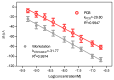
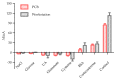
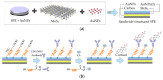
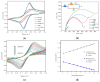
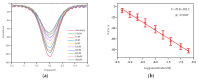
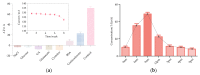
Cortisol is commonly used as a significant biomarker of psychological or physical stress. With the accelerated pace of life, non-invasive cortisol detection at the point of care (POC) is in high demand for personal health monitoring. In this paper, an ultrasensitive immunosensor using gold nanoparticles/molybdenum disulfide/gold nanoparticles (AuNPs/MoS2/AuNPs) as transducer was explored for non-invasive salivary cortisol monitoring at POC with the miniaturized differential pulse voltammetry (DPV) system based on a smartphone. Covalent binding of cortisol antibody (CORT-Ab) onto the AuNPs/MoS2/AuNPs transducer was achieved through the self-assembled monolayer of specially designed polyethylene glycol (PEG, SH-PEG-COOH). Non-specific binding was avoided by passivating the surface with ethanolamine. The miniaturized portable DPV system was utilized for human salivary cortisol detection. A series current response of different cortisol concentrations decreased and exhibited a linear range of 0.5-200 nM, the detection limit of 0.11 nM, and high sensitivity of 30 μA M-1 with a regression coefficient of 0.9947. Cortisol was also distinguished successfully from the other substances in saliva. The recovery ratio of spiked human salivary cortisol and the variation of salivary cortisol level during one day indicated the practicability of the immunosensor based on the portable system. The results demonstrated the excellent performance of the smartphone-based immunosensor system and its great potential application for non-invasive human salivary cortisol detection at POC.
Keywords: differential pulse voltammetry; gold nanoparticles; immunosensor; molybdenum disulfide; salivary cortisol; smartphone.
Conflict of interest statement
The authors declare no conflict of interest.
Figures


References
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

