Hepatotoxicity and Liver-Related Mortality in Women of Childbearing Potential Living With Human Immunodeficiency Virus and High CD4 Cell Counts Initiating Efavirenz-Containing Regimens
- PMID: 32161944
- PMCID: PMC8075031
- DOI: 10.1093/cid/ciaa244
Hepatotoxicity and Liver-Related Mortality in Women of Childbearing Potential Living With Human Immunodeficiency Virus and High CD4 Cell Counts Initiating Efavirenz-Containing Regimens
Abstract
Background: Severe hepatotoxicity in people with human immunodeficiency virus (HIV) receiving efavirenz (EFV) has been reported. We assessed the incidence and risk factors of hepatotoxicity in women of childbearing age initiating EFV-containing regimens.
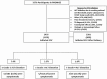
Methods: In the Promoting Maternal and Infant Survival Everywhere (PROMISE) trial, ART-naive pregnant women with HIV and CD4 count ≥ 350 cells/μL and alanine aminotransferase ≤ 2.5 the upper limit of normal were randomized during the antepartum and postpartum periods to antiretroviral therapy (ART) strategies to assess HIV vertical transmission, safety, and maternal disease progression. Hepatotoxicity was defined per the Division of AIDS Toxicity Tables. Cox proportional hazards models were constructed with covariates including participant characteristics, ART regimens, and timing of EFV initiation.
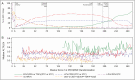
Results: Among 3576 women, 2435 (68%) initiated EFV at a median 121.1 weeks post delivery. After EFV initiation, 2.5% (61/2435) had severe (grade 3 or higher) hepatotoxicity with an incidence of 2.3 (95% confidence interval [CI], 2.0-2.6) per 100 person-years. Events occurred between 1 and 132 weeks postpartum. Of those with severe hepatotoxicity, 8.2% (5/61) were symptomatic, and 3.3% (2/61) of those with severe hepatotoxicity died from EFV-related hepatotoxicity, 1 of whom was symptomatic. The incidence of liver-related mortality was 0.07 (95% CI, .06-.08) per 100 person-years. In multivariable analysis, older age was associated with severe hepatotoxicity (adjusted hazard ratio per 5 years, 1.35 [95% CI, 1.06-1.70]).
Conclusions: Severe hepatotoxicity after EFV initiation occurred in 2.5% of women and liver-related mortality occurred in 3% of those with severe hepatotoxicity. The occurrence of fatal events underscores the need for safer treatments for women of childbearing age.
Keywords: HIV; hepatotoxicity; liver enzyme elevation; real-world.
© The Author(s) 2020. Published by Oxford University Press for the Infectious Diseases Society of America. All rights reserved. For permissions, e-mail: journals.permissions@oup.com.
Figures
References
-
- Sulkowski MS, Thomas DL, Mehta SH, Chaisson RE, Moore RD. Hepatotoxicity associated with nevirapine or efavirenz-containing antiretroviral therapy: role of hepatitis C and B infections. Hepatology 2002; 35:182–9. - PubMed
-
- Stern JO, Robinson PA, Love J, Lanes S, Imperiale MS, Mayers DL. A comprehensive hepatic safety analysis of nevirapine in different populations of HIV infected patients. J Acquir Immune Defic Syndr 2003; 34(Suppl 1):S21–33. - PubMed
-
- Sanne I, Mommeja-Marin H, Hinkle J, et al. Severe hepatotoxicity associated with nevirapine use in HIV-infected subjects. J Infect Dis 2005; 191:825–9. - PubMed
-
- Shubber Z, Calmy A, Andrieux-Meyer I, et al. Adverse events associated with nevirapine and efavirenz-based first-line antiretroviral therapy: a systematic review and meta-analysis. AIDS 2013; 27:1403–12. - PubMed
-
- Hoffmann CJ, Charalambous S, Thio CL, et al. Hepatotoxicity in an African antiretroviral therapy cohort: the effect of tuberculosis and hepatitis B. AIDS 2007; 21:1301–8. - PubMed

