Cerebral palsy with dislocated hip and scoliosis: what to deal with first?
- PMID: 32165978
- PMCID: PMC7043124
- DOI: 10.1302/1863-2548.14.190099
Cerebral palsy with dislocated hip and scoliosis: what to deal with first?
Abstract
Purpose: Hip dislocation and scoliosis are common in children with cerebral palsy (CP). Hip dislocation develops in 15% and 20% of children with CP, mainly between three and six years of age and especially in the spastic and dyskinetic subtypes. The risk of scoliosis increases with age and increasing disability as expressed by the Gross Motor Function Score.
Methods: A hip surveillance programme and early surgical treatment have been shown to reduce the hip dislocation, but it remains unclear if a similar programme could reduce the need for neuromuscular scoliosis. When hip dislocation and neuromuscular scoliosis are co-existent, there appears to be no clear guidelines as to which of these deformities should be addressed first: hip or spine.
Results: Hip dislocation or windswept deformity may cause pelvic obliquity and initiate scoliosis, while neuromuscular scoliosis itself leads to pelvic obliquity and may increase the risk of hip dislocation especially on the high side. It remains unclear if treating imminent hip dislocation can prevent development of scoliosis and vice versa, but they may present at the same time for surgery. Current expert opinion suggests that when hip dislocation and scoliosis present at the same time, scoliosis associated pelvic obliquity should be corrected before hip reconstruction. If the patient is not presenting with pelvic obliquity the more symptomatic condition should be addressed first.
Conclusion: Early identification of hip displacement and neuromuscular scoliosis appears to be important for better surgical outcomes.
Keywords: CP surveillance; cerebral palsy; hip dislocation; hip reconstruction; neuromuscular scoliosis; spinal fusion surgery.
Copyright © 2020, The author(s).
Figures

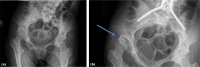
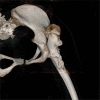
References
-
- Hägglund G, Andersson S, Düppe H, et al. . Prevention of dislocation of the hip in children with cerebral palsy. The first ten years of a population-based prevention programme. J Bone Joint Surg [Br] 2005;87-B:95-101. - PubMed
-
- Soo B, Howard JJ, Boyd RN, et al. . Hip displacement in cerebral palsy. J Bone Joint Surg [Am] 2006;88-A:121-129. - PubMed
-
- Letts M, Shapiro L, Mulder K, Klassen O. The windblown hip syndrome in total body cerebral palsy. J Pediatr Orthop 1984;4:55-62. - PubMed
-
- Senaran H, Shah SA, Glutting JJ, Dabney KW, Miller F. The associated effects of untreated unilateral hip dislocation in cerebral palsy scoliosis. J Pediatr Orthop 2006;26:769-772. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Miscellaneous

