Optimizing Tele-ICU Operational Efficiency Through Workflow Process Modeling and Restructuring
- PMID: 32166245
- PMCID: PMC7063929
- DOI: 10.1097/CCE.0000000000000064
Optimizing Tele-ICU Operational Efficiency Through Workflow Process Modeling and Restructuring
Abstract
Little is known on how to best prioritize various tele-ICU specific tasks and workflows to maximize operational efficiency. We set out to: 1) develop an operational model that accurately reflects tele-ICU workflows at baseline, 2) identify workflow changes that optimize operational efficiency through discrete-event simulation and multi-class priority queuing modeling, and 3) implement the predicted favorable workflow changes and validate the simulation model through prospective correlation of actual-to-predicted change in performance measures linked to patient outcomes.
Setting: Tele-ICU of a large healthcare system in New York State covering nine ICUs across the spectrum of adult critical care.
Patients: Seven-thousand three-hundred eighty-seven adult critically ill patients admitted to a system ICU (1,155 patients pre-intervention in 2016Q1 and 6,232 patients post-intervention 2016Q3 to 2017Q2).
Interventions: Change in tele-ICU workflow process structure and hierarchical process priority based on discrete-event simulation.
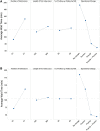
Measurements and main results: Our discrete-event simulation model accurately reflected the actual baseline average time to first video assessment by both the tele-ICU intensivist (simulated 132.8 ± 6.7 min vs 132 ± 12.2 min actual) and the tele-ICU nurse (simulated 128.4 ± 7.6 min vs 123 ± 9.8 min actual). For a simultaneous priority and process change, the model simulated a reduction in average TVFA to 51.3 ± 1.6 min (tele-ICU intensivist) and 50.7 ± 2.1 min (tele-ICU nurse), less than the added simulated reductions for each change alone, suggesting correlation of the changes to some degree. Subsequently implementing both changes simultaneously resulted in actual reductions in average time to first video assessment to values within the 95% CIs of the simulations (50 ± 5.5 min for tele-intensivists and 49 ± 3.9 min for tele-nurses).
Conclusions: Discrete-event simulation can accurately predict the effects of contemplated multidisciplinary tele-ICU workflow changes. The value of workflow process and task priority modeling is likely to increase with increasing operational complexities and interdependencies.
Keywords: modeling; operations research; outcomes; queueing theory; tele-intensive care unit; workflow efficiency.
Copyright © 2019 The Authors. Published by Wolters Kluwer Health, Inc. on behalf of the Society of Critical Care Medicine.
Conflict of interest statement
The authors have disclosed that they do not have any potential conflicts of interest.
Figures


References
-
- Lilly CM, Zubrow MT, Kempner KM, et al. ; Society of Critical Care Medicine Tele-ICU Committee Critical care telemedicine: Evolution and state of the art. Crit Care Med 2014422429–2436 - PubMed
-
- New England Healthcare Institute Massachusetts Technology Collaborative. Critical Care, Critical Choices: The Case for Tele-ICUs in Intensive Care. 2010. Available at: https://www.nehi.net/writable/publication_files/file/teleicu_critical_ca.... Accessed November 27, 2019.
-
- Lilly CM, Fisher KA, Ries M, et al. A national ICU telemedicine survey: Validation and results. Chest 201214240–47 - PubMed
-
- Angus DC, Kelley MA, Schmitz RJ, et al. ; Committee on Manpower for Pulmonary and Critical Care Societies (COMPACCS) Caring for the critically ill patient. Current and projected workforce requirements for care of the critically ill and patients with pulmonary disease: Can we meet the requirements of an aging population? JAMA 20002842762–2770 - PubMed
LinkOut - more resources
Full Text Sources

