Tuberculosis in HIV-Associated Cryptococcal Meningitis is Associated with an Increased Risk of Death
- PMID: 32183112
- PMCID: PMC7141367
- DOI: 10.3390/jcm9030781
Tuberculosis in HIV-Associated Cryptococcal Meningitis is Associated with an Increased Risk of Death
Abstract
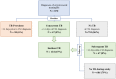
Tuberculosis (TB) and cryptococcal meningitis are leading causes of morbidity and mortality in advanced HIV disease. Data are limited on TB co-infection among individuals with cryptococcal meningitis. We performed a retrospective analysis of HIV-infected participants with cryptococcal meningitis from 2010-2017. Baseline demographics were compared between three groups: 'prevalent TB' if TB treated >14 days prior to cryptococcal meningitis diagnosis, 'concurrent TB' if TB treated ± 14 days from diagnosis, or 'No TB at baseline'. We used time-updated proportional-hazards regression models to assess TB diagnosis as a risk for death. Of 870 participants with cryptococcal meningitis, 50 (6%) had prevalent TB, 67 (8%) had concurrent TB, and 753 (86%) had no baseline TB. Among participants without baseline TB, 67 (9%) were diagnosed with incident TB (after >14 days), with a median time to TB incidence of 41 days (IQR, 22-69). The 18-week mortality was 50% (25/50) in prevalent TB, 46% (31/67) in concurrent TB, and 45% (341/753) in the no TB group (p = 0.81). However, TB co-infection was associated with an increased hazard of death (HR = 1.75; 95% CI, 1.33-2.32; p < 0.001) in a time-updated model. TB is commonly diagnosed in cryptococcal meningitis, and the increased mortality associated with co-infection is a public health concern.
Keywords: AIDS-related opportunistic infections; Cryptococcus; HIV; Tuberculosis; co-infection; cryptococcal meningitis.
Conflict of interest statement
Authors declare no conflicts of interest.
Figures
References
-
- Rajasingham R., Smith R.M., Park B.J., Jarvis J.N., Govender N.P., Chiller T.M., Denning D.W., Loyse A., Boulware D.R. Global burden of disease of HIV-associated cryptococcal meningitis: an updated analysis. Lancet Infect. Dis. 2017;17:873–881. doi: 10.1016/S1473-3099(17)30243-8. - DOI - PMC - PubMed
-
- The Joint United Nations Programme on HIV and AIDS Global HIV & AIDS Statistics-2019 Fact Sheet. [(accessed on 10 August 2019)]; Available online: https://www.unaids.org/en/resources/fact-sheet.
-
- Cox J.A., Lukande R.L., Nelson A.M., Mayanja-Kizza H., Colebunders R., Van Marck E., Manabe Y.C. An autopsy study describing causes of death and comparing clinico-pathological findings among hospitalized patients in Kampala, Uganda. PLoS ONE. 2012;7:e33685. doi: 10.1371/journal.pone.0033685. - DOI - PMC - PubMed
-
- Karat A.S., Omar T., von Gottberg A., Tlali M., Chihota V.N., Churchyard G.J., Fielding K.L., Johnson S., Martinson N.A., McCarthy K., et al. Autopsy Prevalence of Tuberculosis and Other Potentially Treatable Infections among Adults with Advanced HIV Enrolled in Out-Patient Care in South Africa. PLoS ONE. 2016;11:e0166158. doi: 10.1371/journal.pone.0166158. - DOI - PMC - PubMed
Grants and funding
LinkOut - more resources
Full Text Sources

