Impact of reperfusion with blood venting on liver transplantation outcomes; a prospective case-control study
- PMID: 32190225
- PMCID: PMC7069539
Impact of reperfusion with blood venting on liver transplantation outcomes; a prospective case-control study
Abstract
Aim: This study aimed to evaluate the impact of two different reperfusion techniques on outcomes of LT patients.
Background: Post-reperfusion syndrome (PRS) during liver transplantation (LT) remains a serious issue for both the surgeon and anesthetist.
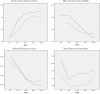
Methods: In this prospective study, all liver transplant recipients referred to the liver transplantation department of Imam Khomeini Hospital, Tehran, Iran, from January 2016 to June 2017 were enrolled in the study and were divided into two groups of vented (reperfusion with 300cc blood venting) and non-vented (reperfusion without blood venting) cases. Then, 30-minute intraoperative hemodynamic and biochemical changes, as well as 2-month complications and 6-month mortality, were compared between the groups.
Results: 57 LT cases (31 vented and 26 non-vented) were studied (50.9% female). The two groups had a similar age (p = 0.107), sex (p = 0.885), MELD score (p = 0.61), donor warm ischemic time (p = 0.85), recipient warm ischemic time (p = 0.36), cold ischemic time (p = 0.99), comorbid disease (p = 0.502), and etiology of end-stage liver disease (p = 0.281). PRS occurred in 3 (11.5%) patients in the vented group and 4 (12.9%) in the non-vented group (p = 0.69). One (3.8%) patient in the non-vented group and 4 (12.9%) patients in vented group died (p = 0.229).
Conclusion: Reperfusion with and without blood venting had the same outcome regarding intraoperative hemodynamic and biochemical changes, PRS rate, and postoperative complications, as well as 6-month survival. Thus, it seems that blood venting is not a necessary method for decreasing post-reperfusion complications following LT.
Keywords: Liver transplantation; Mean arterial pressure; Reperfusion.
©2020 RIGLD, Research Institute for Gastroenterology and Liver Diseases.
Figures
References
-
- Valentine E, Gregorits M, Gutsche JT, Al-Ghofaily L, Augoustides JG. Clinical update in liver transplantation. J Cardiothorac Vasc Anesth. 2013;27:809–15. - PubMed
-
- Reich DL, Wood Jr RK, Emre S, Bodian CA, Hossain S, Krol M, et al. Association of intraoperative hypotension and pulmonary hypertension with adverse outcomes after orthotopic liver transplantation. J Cardiothorac Vasc Anesth. 2003;17:699–702. - PubMed
-
- Aggarwal S. Postreperfusion syndrome: cardiovascular collapse following hepatic reperfusion during liver transplantation. Transplant Proc. 1987;19:54–5. - PubMed
LinkOut - more resources
Full Text Sources