Outcomes of pars plana vitrectomy with subretinal tissue plasminogen activator injection and pneumatic displacement of fovea-involving submacular haemorrhage
- PMID: 32201733
- PMCID: PMC7076260
- DOI: 10.1136/bmjophth-2019-000394
Outcomes of pars plana vitrectomy with subretinal tissue plasminogen activator injection and pneumatic displacement of fovea-involving submacular haemorrhage
Abstract
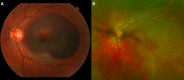
Objective: Fovea-involving subretinal haemorrhage is challenging to manage with uncertain visual outcomes. We reviewed outcomes of patients with fovea-involving macular haemorrhage treated with pars plana vitrectomy (PPV) and subretinal tissue plasminogen activator (tPA) with pneumatic displacement.
Methods and analysis: This is a retrospective interventional case series. All patients with submacular haemorrhage who underwent PPV with subretinal tPA injection were included. Reasons for exclusion encompassed patients who underwent intravitreal tPA injection in the office without surgery, insufficient follow-up or documentation. Primary outcomes of interest were postoperative visual acuity (VA) at month 1 and 3. Secondary outcomes were median VA at month 3 by location of haemorrhage and underlying diagnosis.
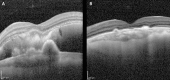
Results: Thirty-seven total patients were included. The mean age was 68.2 years, with 54.1% (20/37) females. The most common aetiology was exudative macular degeneration (43.2%), followed by undifferentiated choroidal neovascularisation (CNV) (18.9%), polypoidal choroidal vasculopathy (18.9%), traumatic CNV (10.8%), macroaneurysm (5.4%) and proliferative diabetic retinopathy (2.7%). Median preoperative VA was 20/2000, postoperative month 1 was 20/347 (p<0.01), improving to 20/152 (p<0.01) at month 3. Proportion of patients gaining vision 3+ lines in vision was 15/36 (42%). Mean preoperative central subfield thickness on optical coherence tomography was 512.2 µm for sub-retinal pigment epithelium haemorrhage and 648.2 µm for subretinal haemorrhage (p=0.48). Difference in VA by diagnosis was not significant (p=0.60).
Conclusions: PPV with subretinal tPA injection and pneumatic displacement of submacular haemorrhage offers modest visual recovery for a diverse group of patients. Location of haemorrhage or specific diagnosis may not predict outcome.
Keywords: macula; neovascularisation; retina; treatment surgery.
© Author(s) (or their employer(s)) 2020. Re-use permitted under CC BY-NC. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
Competing interests: RBR reports consulting fees from Optovue, Boehringer- Ingelheim, NanoRetina, Bayer, Regeneron, CellView, and Astellas. He holds patents with Optovue and has a personal financial interest in Opticology and Guardion Health. None of the other authors report any relevant conflicts or proprietary interest in the results of this study.
Figures
References
LinkOut - more resources
Full Text Sources
Miscellaneous
