Impact of preoperative chemoradiotherapy using concurrent S-1 and CPT-11 on long-term clinical outcomes in locally advanced rectal cancer
- PMID: 32206181
- PMCID: PMC7081115
- DOI: 10.4251/wjgo.v12.i3.311
Impact of preoperative chemoradiotherapy using concurrent S-1 and CPT-11 on long-term clinical outcomes in locally advanced rectal cancer
Abstract
Background: Preoperative chemoradiotherapy regimens using a second drug for locally advanced rectal cancer are still under clinical investigation.
Aim: To investigate the clinical outcomes of patients with locally advanced rectal cancer treated with preoperative chemoradiotherapy using tegafur/gimeracil/oteracil (S-1) plus irinotecan (CPT-11).
Methods: This was a single-center retrospective study of 82 patients who underwent radical surgery for rectal cancer after chemoradiotherapy with S-1 (80 mg/m2/d), CPT-11 (60 mg/m2/d), and radiation (total 45 Gy) between 2009 and 2016. The median follow-up was 51 mo (range: 17-116 mo).
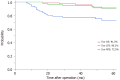
Results: Twenty-nine patients (35.4%) had T3 or T4 rectal cancer with mesorectal fascia invasion, 36 (43.9%) had extramural vascular invasion, 24 (29.8%) had N2 rectal cancer and eight (9.8%) had lateral lymph node swelling. The relative dose intensity was 90.1% for S-1 and 92.9% for CPT-11. Seventy-nine patients (96.3%) underwent R0 resection. With regard to pathological response, 13 patients (15.9%) had a pathological complete response and 52 (63.4%) a good response (tumor regression grade 2/3). The 5-year local recurrence-free survival, relapse-free survival and overall survival rates were 90.1%, 72.5% and 91.3%, respectively. We analyzed the risk factors for local recurrence-free survival by Cox regression analysis and none were detected. Previously described risk factors such as T4 stage, mesorectal fascia invasion or lateral lymph node swelling were not detected as negative factors for local recurrence-free survival.
Conclusion: We demonstrated good compliance and favorable tumor regression in patients with locally advanced rectal cancer treated with preoperative S-1 and CPT-11.
Keywords: Irinotecan; Neoadjuvant chemoradiotherapy; Preoperative chemoradiotherapy; Radiation therapy; Rectal cancer; Tegafur/gimeracil/oteracil.
©The Author(s) 2019. Published by Baishideng Publishing Group Inc. All rights reserved.
Conflict of interest statement
Conflict-of-interest statement: The authors have no conflicts of interest to declare.
Figures
Similar articles
-
UGT1A1 polymorphisms in rectal cancer associated with the efficacy and toxicity of preoperative chemoradiotherapy using irinotecan.Cancer Sci. 2018 Dec;109(12):3934-3942. doi: 10.1111/cas.13807. Epub 2018 Oct 22. Cancer Sci. 2018. PMID: 30246377 Free PMC article.
-
[Analysis on efficacy and safety of total neoadjuvant therapy in patients with locally advanced rectal cancer with high risk factors].Zhonghua Wei Chang Wai Ke Za Zhi. 2019 Apr 25;22(4):349-356. doi: 10.3760/cma.j.issn.1671-0274.2019.04.007. Zhonghua Wei Chang Wai Ke Za Zhi. 2019. PMID: 31054549 Chinese.
-
[Rectum-preserving surgery after consolidation neoadjuvant therapy or totally neoadjuvant therapy for low rectal cancer: a preliminary report].Zhonghua Wei Chang Wai Ke Za Zhi. 2020 Mar 25;23(3):281-288. doi: 10.3760/cma.j.cn.441530-20200228-00096. Zhonghua Wei Chang Wai Ke Za Zhi. 2020. PMID: 32192308 Chinese.
-
Preoperative chemoradiotherapy with oxaliplatin and tegafur-uracil in locally advanced rectal cancer: pathologic complete response rate and preliminary results of overall and disease-free survival in a single institute in Taiwan.J Chin Med Assoc. 2014 Mar;77(3):128-32. doi: 10.1016/j.jcma.2013.11.008. Epub 2014 Jan 4. J Chin Med Assoc. 2014. PMID: 24398439
-
Recent advances in neoadjuvant chemoradiotherapy in locally advanced rectal cancer.J Anus Rectum Colon. 2018 May 25;1(2):39-44. doi: 10.23922/jarc.2017-005. eCollection 2017. J Anus Rectum Colon. 2018. PMID: 31583299 Free PMC article. Review.
Cited by
-
Radiosensitizing Effects of Irinotecan versus Oxaliplatin Alone and in Combination with 5-Fluorouracil on Human Colorectal Cancer Cells.Int J Mol Sci. 2023 Jun 20;24(12):10385. doi: 10.3390/ijms241210385. Int J Mol Sci. 2023. PMID: 37373535 Free PMC article.
-
A single-center retrospective analysis of the efficacy and safety of a modified regimen of irinotecan plus S-1 (IRIS) with molecular targeting agents as second-line chemotherapy in Japanese patients with recurrent or nonresectable colorectal cancer.J Gastrointest Oncol. 2023 Apr 29;14(2):663-675. doi: 10.21037/jgo-22-899. Epub 2023 Apr 10. J Gastrointest Oncol. 2023. PMID: 37201062 Free PMC article.
References
-
- Sauer R, Liersch T, Merkel S, Fietkau R, Hohenberger W, Hess C, Becker H, Raab HR, Villanueva MT, Witzigmann H, Wittekind C, Beissbarth T, Rödel C. Preoperative versus postoperative chemoradiotherapy for locally advanced rectal cancer: results of the German CAO/ARO/AIO-94 randomized phase III trial after a median follow-up of 11 years. J Clin Oncol. 2012;30:1926–1933. - PubMed
-
- Park JH, Yoon SM, Yu CS, Kim JH, Kim TW, Kim JC. Randomized phase 3 trial comparing preoperative and postoperative chemoradiotherapy with capecitabine for locally advanced rectal cancer. Cancer. 2011;117:3703–3712. - PubMed
-
- Glimelius B, Holm T, Blomqvist L. Chemotherapy in addition to preoperative radiotherapy in locally advanced rectal cancer - a systematic overview. Rev Recent Clin Trials. 2008;3:204–211. - PubMed
-
- Taylor FG, Quirke P, Heald RJ, Moran BJ, Blomqvist L, Swift IR, Sebag-Montefiore D, Tekkis P, Brown G Magnetic Resonance Imaging in Rectal Cancer European Equivalence Study Study Group. Preoperative magnetic resonance imaging assessment of circumferential resection margin predicts disease-free survival and local recurrence: 5-year follow-up results of the MERCURY study. J Clin Oncol. 2014;32:34–43. - PubMed
-
- Smith NJ, Barbachano Y, Norman AR, Swift RI, Abulafi AM, Brown G. Prognostic significance of magnetic resonance imaging-detected extramural vascular invasion in rectal cancer. Br J Surg. 2008;95:229–236. - PubMed
LinkOut - more resources
Full Text Sources