Renin-angiotensin-aldosterone system blockade is associated with higher risk of contrast-induced acute kidney injury in patients with diabetes
- PMID: 32241961
- PMCID: PMC7185147
- DOI: 10.18632/aging.102982
Renin-angiotensin-aldosterone system blockade is associated with higher risk of contrast-induced acute kidney injury in patients with diabetes
Abstract
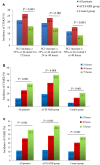
As the incidence of diabetes and cardiovascular comorbidities continues to rise, driven by increased prevalence of obesity and an aging population, so does the demand for percutaneous coronary intervention (PCI) to restore cardiac blood flow. Renin-angiotensin-aldosterone system (RAAS) inhibitors are commonly prescribed to hypertensive diabetic patients to prevent diabetic nephropathy. However, evidence suggests that angiotensin-converting enzyme inhibitors (ACEIs) and angiotensin receptor blockers (ARBs) may increase the risk of contrast-induced acute kidney injury (CIAKI) following coronary angiography (CAG) and PCI. We therefore conducted a retrospective, multicenter study applying the propensity score matching method to evaluate the impact of RAAS inhibition on CIAKI in diabetic patients undergoing CAG/PCI. Among 2240 subjects that met the inclusion criteria, 704 patients in the ACEIs/ARBs group were successfully matched to eligible control patients. The incidence of CIAKI (serum creatinine increase ≥0.5 mg/dl or ≥25% from baseline within 72 h post-CAG/PCI) was significantly higher in the ACEIs/ARBs group than in the control group (26.6% vs. 16.2%, P<0.001). However, control patients showed increased risk of overall adverse cardiovascular events (4.1% vs. 1.8% for ACEIs/ARBs; P=0.016). These data indicate that RAAS inhibition increases the risk of CIAKI in diabetic patients, but confers protection against early cardiovascular events.
Keywords: angiotensin receptor blockers; angiotensin-converting enzyme inhibitors; contrast-induced acute kidney injury; coronary angiography; diabetes mellitus.
Conflict of interest statement
Figures

References
-
- Morice MC, Serruys PW, Kappetein AP, Feldman TE, Ståhle E, Colombo A, Mack MJ, Holmes DR, Choi JW, Ruzyllo W, Religa G, Huang J, Roy K, et al. Five-year outcomes in patients with left main disease treated with either percutaneous coronary intervention or coronary artery bypass grafting in the synergy between percutaneous coronary intervention with taxus and cardiac surgery trial. Circulation. 2014; 129:2388–94. 10.1161/CIRCULATIONAHA.113.006689 - DOI - PubMed
-
- Farooq V, van Klaveren D, Steyerberg EW, Meliga E, Vergouwe Y, Chieffo A, Kappetein AP, Colombo A, Holmes DR Jr, Mack M, Feldman T, Morice MC, Ståhle E, et al. Anatomical and clinical characteristics to guide decision making between coronary artery bypass surgery and percutaneous coronary intervention for individual patients: development and validation of SYNTAX score II. Lancet. 2013; 381:639–50. 10.1016/S0140-6736(13)60108-7 - DOI - PubMed
-
- Posma RA, Lexis CP, Lipsic E, Nijsten MW, Damman K, Touw DJ, van Veldhuisen DJ, van der Harst P, van der Horst IC. Effect of Metformin on Renal Function After Primary Percutaneous Coronary Intervention in Patients Without Diabetes Presenting with ST-elevation Myocardial Infarction: data from the GIPS-III Trial. Cardiovasc Drugs Ther. 2015; 29:451–59. 10.1007/s10557-015-6618-1 - DOI - PMC - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Medical
Miscellaneous

