Implementing structured team debriefing using a Black Box in the operating room: surveying team satisfaction
- PMID: 32253558
- PMCID: PMC7886753
- DOI: 10.1007/s00464-020-07526-3
Implementing structured team debriefing using a Black Box in the operating room: surveying team satisfaction
Abstract
Background: Surgical safety may be improved using a medical data recorder (MDR) for the purpose of postoperative team debriefing. It provides the team in the operating room (OR) with the opportunity to look back upon their joint performance objectively to discuss and learn from suboptimal situations or possible adverse events. The aim of this study was to investigate the satisfaction of the OR team using an MDR, the OR Black Box®, in the OR as a tool providing output for structured team debriefing.
Methods: In this longitudinal survey study, 35 gastro-intestinal laparoscopic operations were recorded using the OR Black Box® and the output was subsequently debriefed with the operating team. Prior to study, a privacy impact assessment was conducted to ensure alignment with applicable legal and regulatory requirements. A structured debrief model and an OR Back Box® performance report was developed. A standardized survey was used to measure participant's satisfaction with the team debriefing, the debrief model used and the performance report. Factor analysis was performed to assess the questionnaire's quality and identified contributing satisfaction factors. Multivariable analysis was performed to identify variables associated with participants' opinions.
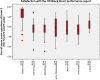
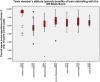
Results: In total, 81 team members of various disciplines in the OR participated, comprising 35 laparoscopic procedures. Mean satisfaction with the OR Black Box® performance report and team debriefing was high for all 3 identified independent satisfaction factors. Of all participants, 98% recommend using the OR Black Box® and the outcome report in team debriefing.
Conclusion: The use of an MDR in the OR for the purpose of team debriefing is considered to be both beneficial and important. Team debriefing using the OR Black Box® outcome report is highly recommended by 98% of team members participating.
Keywords: Black Box; Medical data recorder; Operating room; Surgical safety; Team debriefing; Training.
Conflict of interest statement
Dr. Grantcharov holds intellectual property ownership of Surgical Safety Technologies Inc., is the founder of the OR Black Box®, and is supported by research grants from Medtronic Canada, Ethicon Canada, Baxter Canada, Olympus Canada, Takeda Canada, and Intuitive Canada. Dr. Schijven has no conflict of interest, but was supported by a research grant from Olympus the Netherlands. Dr. Schijven has recently (dec 2019) been appointed as affiliate scientist to the Li Ka Shing Knowledge Insitute of St. Michael’s Hospital, Toronto. Miss van Dalen, Drs. M. Jansen, Drs. van Haperen, Dr. van Dieren, Dr. Buskens, Dr. Nieveen van Dijkum, and Dr. Bemelman have no conflict of interest or financial ties to disclose.
Figures



Similar articles
-
Development of a Model for Video-Assisted Postoperative Team Debriefing.J Surg Res. 2021 Jan;257:625-635. doi: 10.1016/j.jss.2020.07.065. Epub 2020 Sep 17. J Surg Res. 2021. PMID: 32950906 Review.
-
'Herding cats': A mixed methods investigation into the educational value of debriefing in operating theatres.J Perioper Pract. 2024 Jan-Feb;34(1-2):20-25. doi: 10.1177/17504589221149842. Epub 2023 Jan 28. J Perioper Pract. 2024. PMID: 36708282
-
Improvement in student-led debriefing analysis after simulation-based team training using a revised teamwork assessment tool.Surgery. 2021 Dec;170(6):1659-1664. doi: 10.1016/j.surg.2021.06.014. Epub 2021 Jul 28. Surgery. 2021. PMID: 34330538
-
Changing Operating Room Culture: Implementation of a Postoperative Debrief and Improved Safety Culture.World Neurosurg. 2017 Nov;107:597-603. doi: 10.1016/j.wneu.2017.08.090. Epub 2017 Aug 24. World Neurosurg. 2017. PMID: 28843757
-
Debriefing to improve interprofessional teamwork in the operating room: A systematic review.J Nurs Scholarsh. 2023 Nov;55(6):1179-1188. doi: 10.1111/jnu.12924. Epub 2023 Jul 15. J Nurs Scholarsh. 2023. PMID: 37452720
Cited by
-
Smart Operating Room in Digestive Surgery: A Narrative Review.Healthcare (Basel). 2024 Aug 1;12(15):1530. doi: 10.3390/healthcare12151530. Healthcare (Basel). 2024. PMID: 39120233 Free PMC article. Review.
-
Interprofessional staff perspectives on the adoption of or black box technology and simulations to improve patient safety: a multi-methods survey.Adv Simul (Lond). 2023 Oct 25;8(1):24. doi: 10.1186/s41077-023-00263-2. Adv Simul (Lond). 2023. PMID: 37880765 Free PMC article.
-
Creating a Practical Transformational Change Management Model for Novel Artificial Intelligence-Enabled Technology Implementation in the Operating Room.Mayo Clin Proc Innov Qual Outcomes. 2022 Oct 27;6(6):584-596. doi: 10.1016/j.mayocpiqo.2022.09.004. eCollection 2022 Dec. Mayo Clin Proc Innov Qual Outcomes. 2022. PMID: 36324987 Free PMC article.
-
Healthcare professionals' perception of safety culture and the Operating Room (OR) Black Box technology before clinical implementation: a cross-sectional survey.BMJ Open Qual. 2022 Dec;11(4):e001819. doi: 10.1136/bmjoq-2022-001819. BMJ Open Qual. 2022. PMID: 36588330 Free PMC article.
-
Enhancing Surgical Safety and Efficiency: Systematic Review and Single-Arm Meta-Analysis of Surgical Data Recorders.J Med Internet Res. 2025 Jul 28;27:e72703. doi: 10.2196/72703. J Med Internet Res. 2025. PMID: 40720888 Free PMC article.
References
-
- Zegers M, de Bruijne MC, Wagner C, et al. Adverse events and potentially preventable deaths in Dutch hospitals: results of a retrospective patient record review study. Qual Saf Health Care. 2009;18(4):297–302. - PubMed
-
- Makary MA, Daniel M. Medical error—the third leading cause of death in the US. BMJ. 2016 - PubMed
-
- Anderson O, Davis R, Hanna GB, et al. Surgical adverse events: a systematic review. Am J Surg. 2013;206(2):253–262. - PubMed
-
- Rajasekaran S, Ravi S, Aiyer SN. Incidence and preventability of adverse events in an orthopaedic unit: a prospective analysis of four thousand, nine hundred and six admissions. Int Orthop. 2016;40(11):2233–2238. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources

