Association of serum lipoprotein(a) level with the severity and prognosis of calcific aortic valve stenosis: a Chinese cohort study
- PMID: 32280329
- PMCID: PMC7118012
- DOI: 10.11909/j.issn.1671-5411.2020.03.009
Association of serum lipoprotein(a) level with the severity and prognosis of calcific aortic valve stenosis: a Chinese cohort study
Abstract
Background: There was a causal relationship between elevated lipoprotein(a) [Lp(a)] levels and increased risk of calcific aortic valve stenosis (CAVS) in whites and blacks. The present study aimed to investigate whether Lp(a) levels were associated with aortic stenosis (AS) severity and clinical events in Chinese patients.
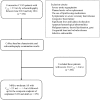
Methods: Levels of serum Lp(a) were measured in 652 patients with CAVS, whom all underwent baseline echocardiographic examination. The clinical endpoint was defined as a composite of aortic valve replacement (AVR) and cardiac death.
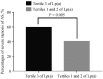
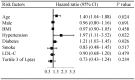
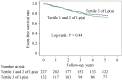
Results: Patients in the tertile 3 of Lp(a) had a higher percentage of severe AS compared with those in the tertile 1 and 2 of Lp(a) (46.2% vs. 33.9%, P = 0.005). Moreover, the top tertile of Lp(a) was an independent predictor of severe AS (OR = 1.78, 95% CI: 1.18-2.66, P = 0.006). However, there was no significant association between tertile 3 of Lp(a) and clinical events (hazard ratio: 0.73; 95% CI: 0.43-1.24; P = 0.239) in the multivariate Cox regression analysis during a mean follow-up time of 3.16 ± 2.74 years.
Conclusions: Elevated Lp(a) level was an independent predictor of severe AS by echocardiography in the Chinese population, but was not associated with the increased risk of AVR and cardiac death, suggesting that Lp(a) levels might be helpful in the risk stratification of patients with CAVS.
Keywords: Aortic stenosis; Calcification; Lipoprotein(a); Prognosis; Severity.
Institute of Geriatric Cardiology.
Figures
Similar articles
-
Impact of Lipoprotein(a) on Valvular and Cardiovascular Outcomes in Patients With Calcific Aortic Valve Stenosis.J Am Heart Assoc. 2025 Mar 18;14(6):e038955. doi: 10.1161/JAHA.124.038955. Epub 2025 Mar 13. J Am Heart Assoc. 2025. PMID: 40079323 Free PMC article.
-
Genetic Variation in LPA, Calcific Aortic Valve Stenosis in Patients Undergoing Cardiac Surgery, and Familial Risk of Aortic Valve Microcalcification.JAMA Cardiol. 2019 Jul 1;4(7):620-627. doi: 10.1001/jamacardio.2019.1581. JAMA Cardiol. 2019. PMID: 31141105 Free PMC article.
-
Association of Mild to Moderate Aortic Valve Stenosis Progression With Higher Lipoprotein(a) and Oxidized Phospholipid Levels: Secondary Analysis of a Randomized Clinical Trial.JAMA Cardiol. 2018 Dec 1;3(12):1212-1217. doi: 10.1001/jamacardio.2018.3798. JAMA Cardiol. 2018. PMID: 30476957 Free PMC article. Clinical Trial.
-
Lipoprotein(a) and calcific aortic valve stenosis: A systematic review.Prog Cardiovasc Dis. 2020 Jul-Aug;63(4):496-502. doi: 10.1016/j.pcad.2020.06.002. Epub 2020 Jun 8. Prog Cardiovasc Dis. 2020. PMID: 32526213
-
The current landscape of lipoprotein(a) in calcific aortic valvular disease.Curr Opin Cardiol. 2021 Sep 1;36(5):542-548. doi: 10.1097/HCO.0000000000000901. Curr Opin Cardiol. 2021. PMID: 34397461 Free PMC article. Review.
Cited by
-
Lipoprotein(a) and Cardiovascular Disease in Chinese Population: A Beijing Heart Society Expert Scientific Statement.JACC Asia. 2022 Nov 15;2(6):653-665. doi: 10.1016/j.jacasi.2022.08.015. eCollection 2022 Nov. JACC Asia. 2022. PMID: 36444328 Free PMC article. Review.
-
Lipoprotein(a) and calcific aortic valve disease initiation and progression: a systematic review and meta-analysis.Cardiovasc Res. 2023 Jul 6;119(8):1641-1655. doi: 10.1093/cvr/cvad062. Cardiovasc Res. 2023. PMID: 37078819 Free PMC article.
References
-
- Nkomo VT, Gardin JM, Skelton TN, et al. Burden of valvular heart diseases: a population-based study. Lancet. 2006;368:1005–1011. - PubMed
-
- Zhao Y, Nicoll R, He YH, et al. The effect of statins on valve function and calcification in aortic stenosis: a meta-analysis. Atherosclerosis. 2016;246:318–324. - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous
