The Clinical Relevance of p16 and p53 Status in Patients with Squamous Cell Carcinoma of the Vulva
- PMID: 32280343
- PMCID: PMC7128067
- DOI: 10.1155/2020/3739075
The Clinical Relevance of p16 and p53 Status in Patients with Squamous Cell Carcinoma of the Vulva
Abstract
Objective: To investigate the prognostic significance of HPV status in vulvar squamous cell carcinomas (VSCC) and to determine whether preoperative determination of p16 or p53 status would have clinical relevance.
Methods: Patients treated for VSCC at a tertiary hospital in Sydney, Australia, from 2002 to 2014, were retrospectively evaluated (n = 119). Histological specimens were stained for p53 and p16 expression, and HPV status was determined by PCR detection of HPV DNA.
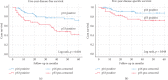
Results: HPV DNA was detected in 19%, p16 expression in 53%, and p53 expression in 37% of patients. Kaplan-Meier survival estimates indicated that p16/HPV-positive patients had superior five-year disease-free survival (76% versus 42%, resp., p = 0.004) and disease-specific survival (DSS) (89% versus 75% resp., p = 0.05) than p53-positive patients. In univariate analysis, nodal metastases (p < 0.001), tumor size >4 cm (p = 0.03), and perineural invasion (p = 0.05) were associated with an increased risk of disease progression and p16 expression with a decreased risk (p = 0.03). In multivariable analysis, only nodal metastases remained independent for risk of disease progression (p = 0.01). For DSS, lymph node metastases (p < 0.001) and tumor size (p = 0.008) remained independently prognostic.
Conclusion: The p16/HPV and p53 status of VSCC allows separation of patients into two distinct clinicopathological groups, although 10% of patients fall into a third group which is HPV, p16, and p53 negative. p16 status was not independently prognostic in multivariable analysis. Treatment decisions should continue to be based on clinical indicators rather than p16 or p53 status.
Copyright © 2020 Ellen L. Barlow et al.
Conflict of interest statement
The authors declare no conflicts of interest regarding the publication of this paper.
Figures
References
LinkOut - more resources
Full Text Sources
Research Materials
Miscellaneous