Value and Feasibility of Telephone Follow-Up in Ethiopian Surgical Patients
- PMID: 32301651
- PMCID: PMC7398427
- DOI: 10.1089/sur.2020.054
Value and Feasibility of Telephone Follow-Up in Ethiopian Surgical Patients
Abstract
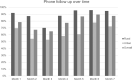
Background: Surgical site infections (SSIs) represent a major cause of morbidity and mortality in Ethiopia. Lack of post-discharge follow-up, including identification of SSIs, is a barrier to continued patient care, often because of financial and travel constraints. As part of a surgical quality improvement initiative, we aimed to assess patient outcomes at 30 days post-operative with a telephone call. Patients and Methods: We conducted mobile telephone follow-up as part of Lifebox's ongoing Clean Cut program, which aims to improve compliance with intra-operative infection prevention standards. One urban tertiary referral hospital and one rural district general hospital in Ethiopia were included in this phase of the study; hospital nursing staff called patients at 30 days post-operative inquiring about signs of SSIs, health-care-seeking behavior, and treatments provided if patients had any healthcare encounters since discharge. Results: A total of 701 patients were included; overall 77% of patients were reached by telephone call after discharge. The rural study site reached 362 patients (87%) by telephone; the urban site reached 176 patients (62%) (p < 0.001). Of the 39 SSIs identified, 19 (49%) were captured as outpatient during the telephone follow-up (p < 0.001); 22 (34%) of all complications were captured following discharge (p < 0.001). Telephone follow-up improved from 65%-78% in the first half of project implementation to 77%-89% in the second half of project implementation. Conclusion: Telephone follow-up after surgery in Ethiopia is feasible and valuable, and identified nearly half of all SSIs and one-third of total complications in our cohort. Follow-up improved over the course of the program, likely indicating a learning curve that, once overcome, is a more accurate marker of its practicability. Given the increasing use of mobile telephones in Ethiopia and ease of implementation, this model could be practical in other low-resource surgical settings.
Keywords: low- and middle-income countries; patient follow-up; surgical outcomes.
Conflict of interest statement
No competing financial interests exist.
Figures
References
-
- Allegranzi B, Bagheri Nejad S, Combescure C, Graafmans W, Attar H, Donaldson L, et al. . Burden of endemic health-care-associated infection in developing countries: Systematic review and meta-analysis. Lancet 2011;377:228–241 - PubMed
-
- Shepard J, Ward W, Milstone A, et al. . Financial impact of surgical site infections on hospitals: The hospital management perspective. JAMA Surg 2013;148:907–914 - PubMed
-
- Jha AK, Larizgoitia I, Audera-Lopez C, et al. . The global burden of unsafe medical care: Analytic modelling of observational studies. BMJ Qual Saf 2013; 22:809–815 - PubMed
-
- Rothe C, Schlaich C, Thompson S. Healthcare-associated infections in sub-Saharan Africa. J Hosp Infect 2013;85:257–267 - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous