Social Determinants of Health and 90-Day Mortality After Hospitalization for Heart Failure in the REGARDS Study
- PMID: 32316807
- PMCID: PMC7428585
- DOI: 10.1161/JAHA.119.014836
Social Determinants of Health and 90-Day Mortality After Hospitalization for Heart Failure in the REGARDS Study
Abstract
Background Outcomes following heart failure (HF) hospitalizations are poor, with 90-day mortality rates of 15% to 20%. Although prior studies found associations between individual social determinants of health (SDOH) and post-discharge mortality, less is known about how an individuals' total burden of SDOH affects 90-day mortality. Methods and Results We included participants of the REGARDS (Reasons for Geographic and Racial Differences in Stroke) Study who were Medicare beneficiaries aged ≥65 years discharged alive after an adjudicated HF hospitalization. Guided by the Healthy People 2020 Framework, we examined 9 SDOH. First, we examined age-adjusted associations between each SDOH and 90-day mortality; those associated with 90-day mortality were used to create an SDOH count. Next, we determined the hazard of 90-day mortality by the SDOH count, adjusting for confounders. Over 10 years, 690 participants were hospitalized for HF at 440 unique hospitals in the United States; there were a total of 79 deaths within 90 days. Overall, 28% of participants had 0 SDOH, 39% had 1, and 32% had ≥2. Compared with those with 0, the age-adjusted hazard ratio for 90-day mortality among those with 1 SDOH was 2.89 (95% CI, 1.46-5.72) and was 3.06 (1.51-6.19) among those with ≥2 SDOH. The adjusted hazard ratio was 2.78 (1.37-5.62) and 2.57 (1.19-5.54) for participants with 1 SDOH and ≥2, respectively. Conclusions While having any of the SDOH studied here markedly increased risk of 90-day mortality after an HF hospitalization, a greater burden of SDOH was not associated with significantly greater risk in our population.
Keywords: cohort study; heart failure; mortality; social determinants of health.
Figures
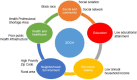

References
-
- Yancy CW, Jessup M, Bozkurt B, Butler J, Casey DE Jr, Drazner MH, Fonarow GC, Geraci SA, Horwich T, Januzzi JL, et al. 2013 ACCF/AHA guideline for the management of heart failure: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. Circulation. 2013;128:e240–e327. - PubMed
-
- Gheorghiade M, Vaduganathan M, Fonarow GC, Bonow RO. Rehospitalization for heart failure: problems and perspectives. J Am Coll Cardiol. 2013;61:391–403. - PubMed
-
- Cheng RK, Cox M, Neely ML, Heidenreich PA, Bhatt DL, Eapen ZJ, Hernandez AF, Butler J, Yancy CW, Fonarow GC. Outcomes in patients with heart failure with preserved, borderline, and reduced ejection fraction in the Medicare population. Am Heart J. 2014;168:721–730. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical
Research Materials
Miscellaneous

