Number of consulting medical institutions and risk of polypharmacy in community-dwelling older people under a healthcare system with free access: a cross-sectional study in Japan
- PMID: 32336271
- PMCID: PMC7183655
- DOI: 10.1186/s12913-020-05205-6
Number of consulting medical institutions and risk of polypharmacy in community-dwelling older people under a healthcare system with free access: a cross-sectional study in Japan
Abstract
Background: Under the Japanese free access healthcare system, patients are allowed to consult multiple medical institutions (including clinics and hospitals for general or specialist consultation) without primary care referral. This potentially increases the risk of polypharmacy. We examined the association between the number of consulting medical institutions and polypharmacy under a healthcare system with free access.
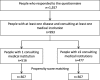
Methods: Via a self-administered questionnaire, we identified people aged ≥65 years with ≥1 disease and ≥1 consulting medical institution in a Japanese city in 2016. The exposure of interest was the number of consulting medical institutions (1, 2, or ≥3) and the outcome was polypharmacy (use of ≥6 types of drugs). We performed a multivariate logistic regression analysis, adjusting for age, sex, household economy, and the number and type of comorbidities. To minimize confounding effects, we also performed propensity-score-matched analysis, categorizing patients into two groups: 1 and ≥2 consulting medical institutions.
Results: Of 993 eligible individuals (mean (standard deviation) age: 75.1 (6.5) years, men: 52.6%), 15.7% (156/993) showed polypharmacy. Proportions of polypharmacy were 9.7% (50/516), 16.6% (55/332), and 35.2% (51/145) for people who consulted 1, 2, and ≥3 medical institutions, respectively. Relative to people who consulted 1 medical institution, adjusted odds ratios (95% confidence intervals) for polypharmacy were 1.50 (0.94-2.37) and 3.34 (1.98-5.65) for those who consulted 2 and ≥3 medical institutions, respectively. In propensity score matching, of 516 and 477 patients who consulted 1 and ≥2 medical institutions, 307 pairs were generated. The proportion of polypharmacy was 10.8% (33/307) and 17.3% (53/307), respectively (P = 0.020). The odds ratio for polypharmacy (≥2 vs. 1 consulting medical institution) was 1.73 (95% confidence interval 1.09-2.76).
Conclusions: Patients who consulted more medical institutions were more likely to show polypharmacy. The results could encourage physicians and pharmacists to collect medication information more actively and conduct appropriate medication reviews. Strengthening primary care is needed to address the polypharmacy issue, especially in countries with healthcare systems with free access.
Keywords: Free access; Multiple consultations; Number of consulting medical institutions; Polypharmacy.
Conflict of interest statement
Nanako Tamiya is Editorial Board Member.
Figures
Similar articles
-
Factors associated with appropriate knowledge of the indications for prescribed drugs among community-dwelling older patients with polypharmacy.Age Ageing. 2016 May;45(3):402-8. doi: 10.1093/ageing/afw045. Epub 2016 Mar 24. Age Ageing. 2016. PMID: 27013501
-
Association between polypharmacy and cognitive impairment in an elderly Japanese population residing in an urban community.Geriatr Gerontol Int. 2017 Sep;17(9):1286-1293. doi: 10.1111/ggi.12862. Epub 2016 Sep 15. Geriatr Gerontol Int. 2017. PMID: 27628036
-
Use of traditional and orthodox health services in urban Zimbabwe.Int J Epidemiol. 1995 Oct;24(5):1006-12. doi: 10.1093/ije/24.5.1006. Int J Epidemiol. 1995. PMID: 8557433
-
Time intervals to care and health service use experiences of uninsured cancer patients treated under public financing in Mexico City.Cancer Epidemiol. 2023 Jun;84:102366. doi: 10.1016/j.canep.2023.102366. Epub 2023 Apr 20. Cancer Epidemiol. 2023. PMID: 37086645 Review.
-
Does Having a Usual Primary Care Provider Reduce Polypharmacy Behaviors of Patients With Chronic Disease? A Retrospective Study in Hubei Province, China.Front Pharmacol. 2022 Jan 21;12:802097. doi: 10.3389/fphar.2021.802097. eCollection 2021. Front Pharmacol. 2022. PMID: 35126137 Free PMC article. Review.
Cited by
-
Community-level social capital and polypharmacy among public assistance recipients in Japan: A multilevel cross-sectional study.SSM Popul Health. 2025 Mar 20;30:101788. doi: 10.1016/j.ssmph.2025.101788. eCollection 2025 Jun. SSM Popul Health. 2025. PMID: 40212734 Free PMC article.
-
Polypharmacy and potentially inappropriate medications in older adults who use long-term care services: a cross-sectional study.BMC Geriatr. 2024 Aug 21;24(1):696. doi: 10.1186/s12877-024-05296-4. BMC Geriatr. 2024. PMID: 39169279 Free PMC article.
-
Association of Self-Reported Medication Adherence with Potentially Inappropriate Medications in Elderly Patients: A Cross-Sectional Pilot Study.Int J Environ Res Public Health. 2020 Aug 16;17(16):5940. doi: 10.3390/ijerph17165940. Int J Environ Res Public Health. 2020. PMID: 32824284 Free PMC article.
-
A narrative review of evidence to guide deprescribing among older adults.J Gen Fam Med. 2021 May 28;22(4):182-196. doi: 10.1002/jgf2.464. eCollection 2021 Jul. J Gen Fam Med. 2021. PMID: 34221792 Free PMC article. Review.
-
Association between smoking habits and dental care utilization and cost using administrative claims database and specific medical check-up data.BMC Oral Health. 2022 Sep 2;22(1):372. doi: 10.1186/s12903-022-02397-7. BMC Oral Health. 2022. PMID: 36056338 Free PMC article.
References
-
- Fushiki Y, Kinoshita K, Tokuda Y. Polypharmacy and adverse drug events leading to acute care hospitalization in Japanese elderly. Gen Med. 2014;15(2):110–116. doi: 10.14442/general.15.110. - DOI
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Medical